
What is population health?
We’re all familiar with our own healthcare needs: We do our best to stay fit and healthy, but sometimes we get sick, we go to the doctor and we get treated. But how does our own health fit into a bigger picture? Are there questions we can answer that allow us to understand the health needs of a population more broadly? Are there questions we should be asking—but aren’t?
Posing these questions, and probing for answers, is the definition of population health.
Population health encourages us to focus on the health outcomes of a group of people, studying the varied factors and patterns at play in determining those outcomes. It is related, yet distinct, from public health. Public health refers to what we do as a society to ensure that people can be healthier. When health officials urge us to get flu shots, they’re acting to protect public health. The term can also be confused with population health management, which refers specifically to the role of technology and data in improving health.
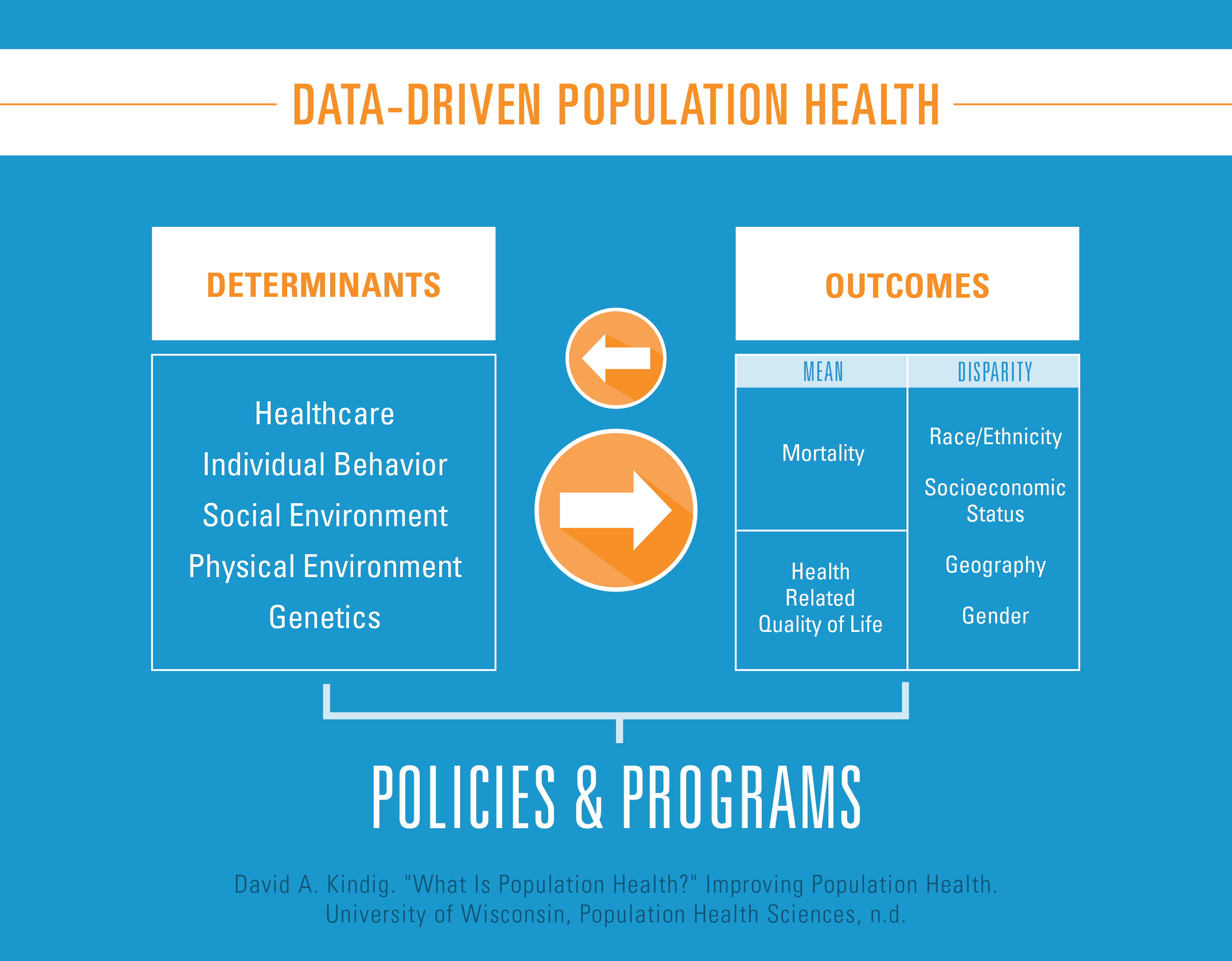
What are health determinants?
Studies show that 70 to 80 percent of health outcomes can be attributed to an individual’s environment and behavior. These social determinants can include everything from neighborhoods and social environments to genetics, education and economic status.
Social determinants can provide clues to a community’s unique needs and risk factors, and help identify the most effective policies or programs to address them. For example, in a city with dramatic spikes in pediatric asthma, it would help to explore whether pollution, housing conditions or access to disease management programs are factors.
How can data help population health?
Data can identify patterns or trends, and help us set priorities for improvement and track changes over time.
Using claims data from more than 40 million individuals, the BCBS Health Index SM tells us that hypertension is the top condition affecting the health of residents in Lincoln, Redwood and Roseau counties of Minnesota.
To address this challenge, Blue Cross Blue Shield of Minnesota (BCBSMN) provides full coverage of hypertension management benefits with no co-pay. This not only removes a financial barrier, but also motivates patients to keep their condition under control by providing disease management training, access to drugs and tests and has improved medication adherence by 2 percent.
In Swain County, NC, where diabetes is a top condition, Blue Cross Blue Shield of North Carolina led a statewide program to increase the number of people screened for diabetes. Using a $15 gift card as an incentive, more than 30 percent of those identified as being at risk for diabetes participated.
In Tennessee, a number of counties affected by depression and anxiety can look to Blue Care Tennessee, a Blue Cross Blue Shield of Tennessee Medicaid plan. The plan is working with the Tennessee Chapter of the American Academy of Pediatrics to give pediatricians the tools they need to improve behavioral health screening rates. Since the program started, 51 percent of participants started using behavioral health screening tools in their practice and 43 percent reported avoiding sending patients with behavioral health concerns to the emergency room.
By using data in these ways and others, we can allocate resources efficiently for the greatest possible impact in improving health.

