Executive Summary
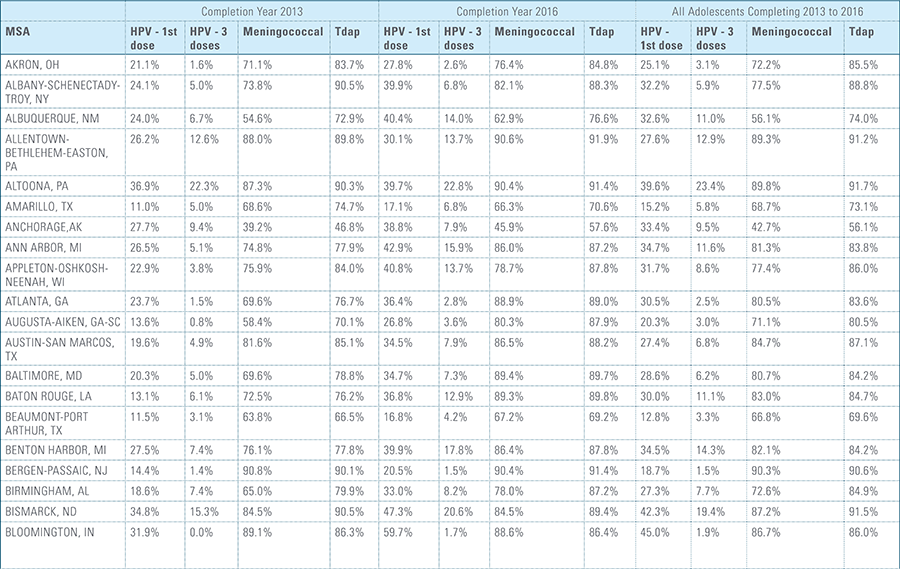
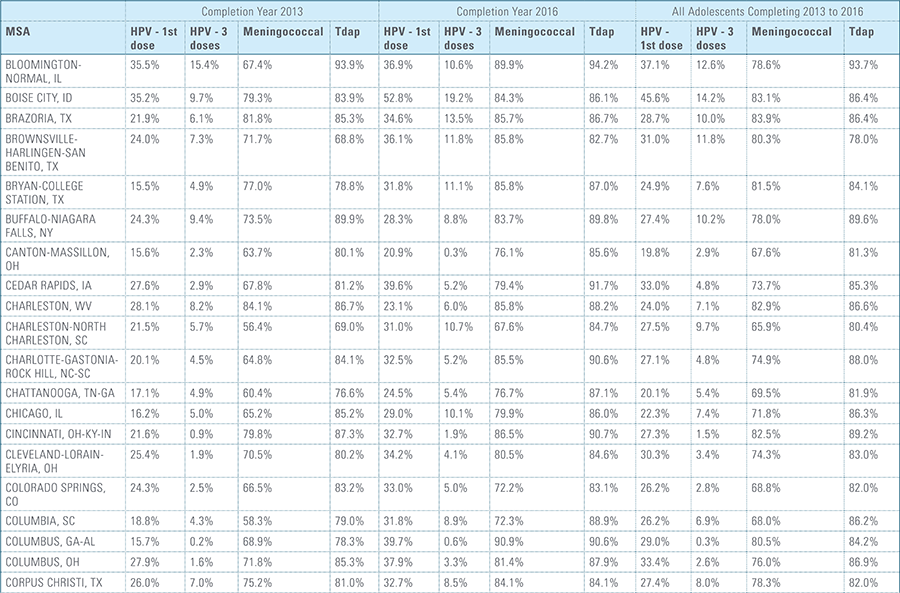
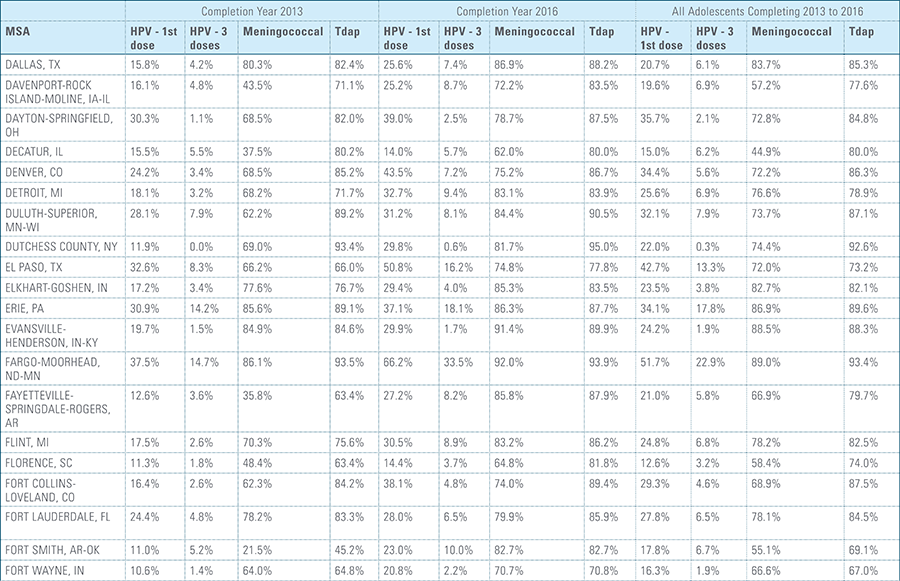
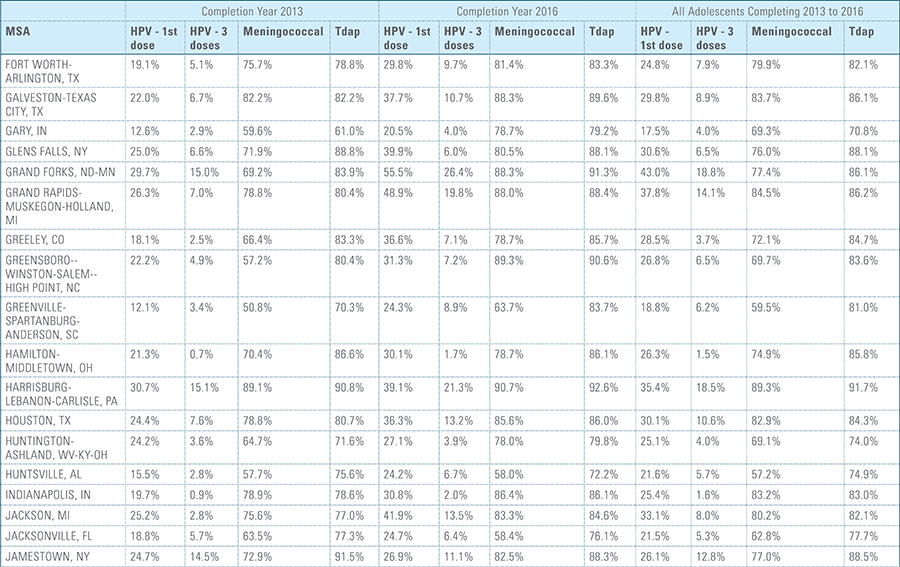
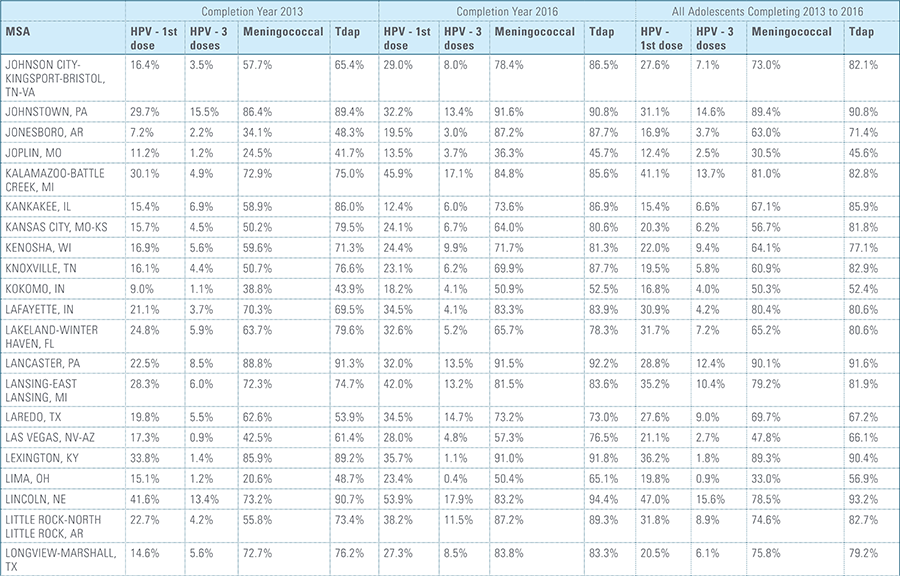
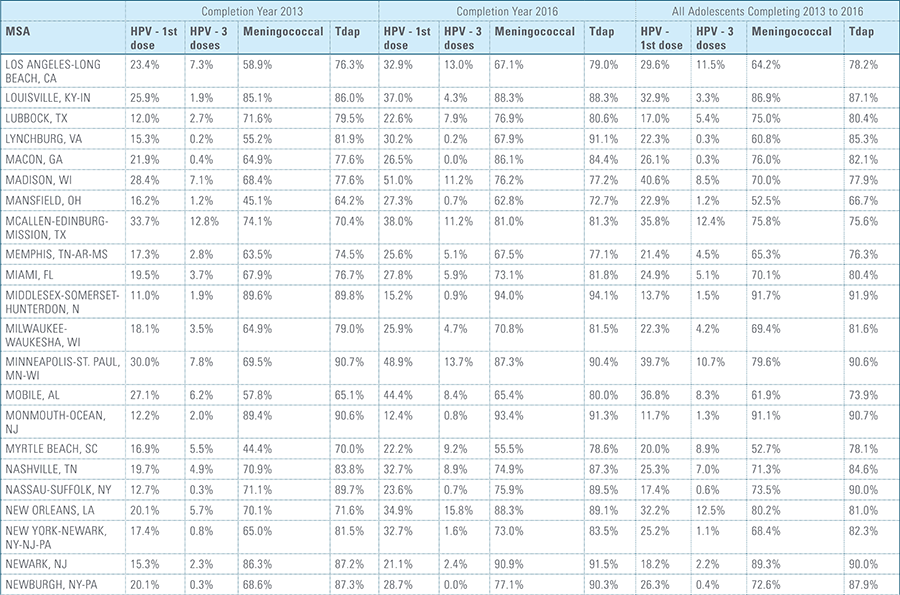
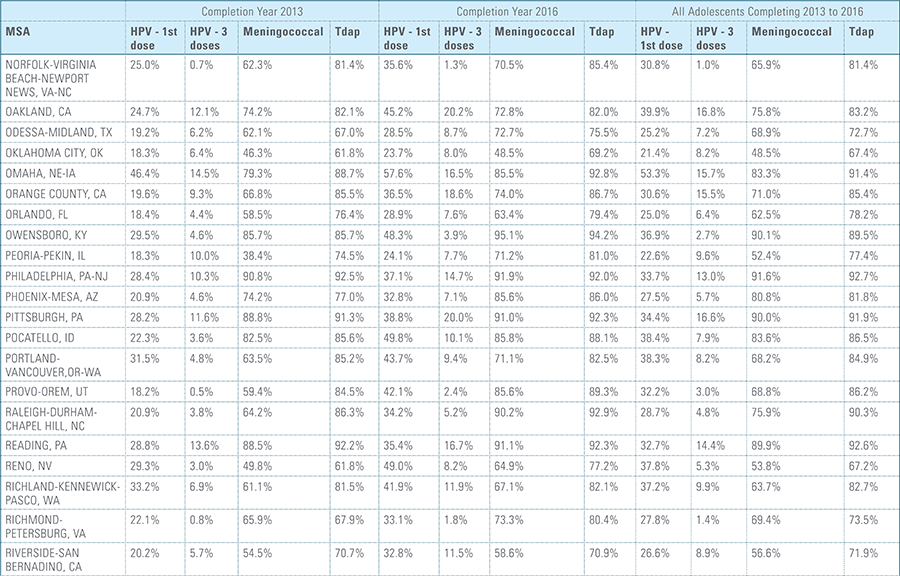
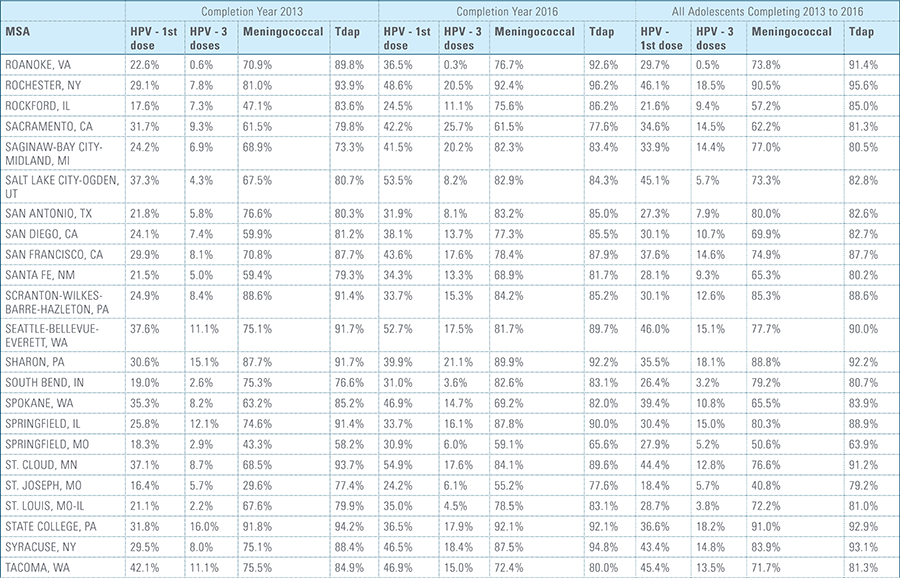
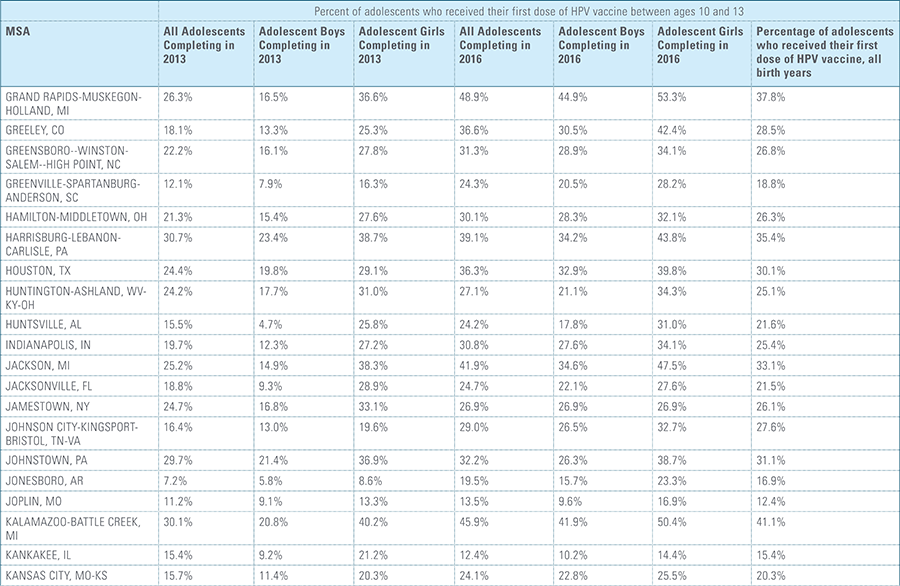
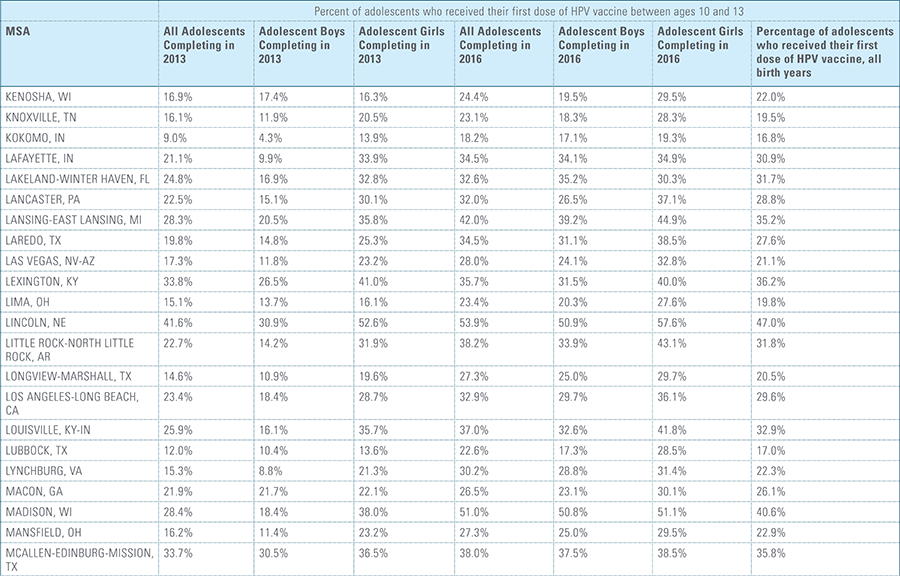
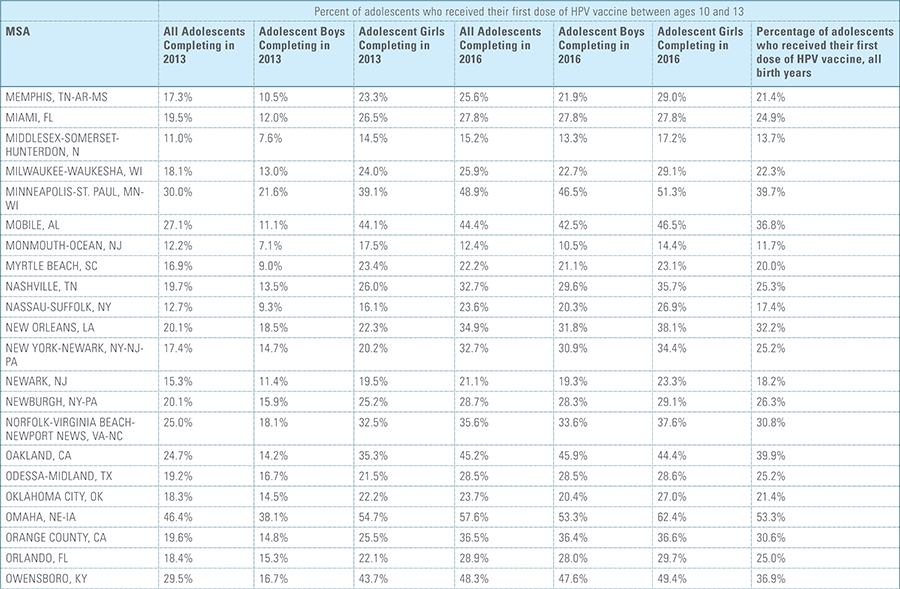
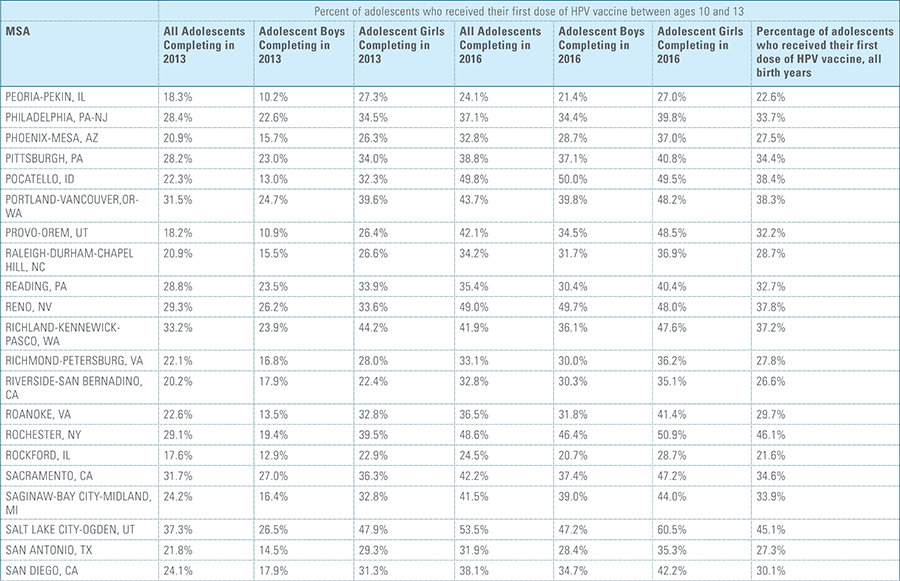
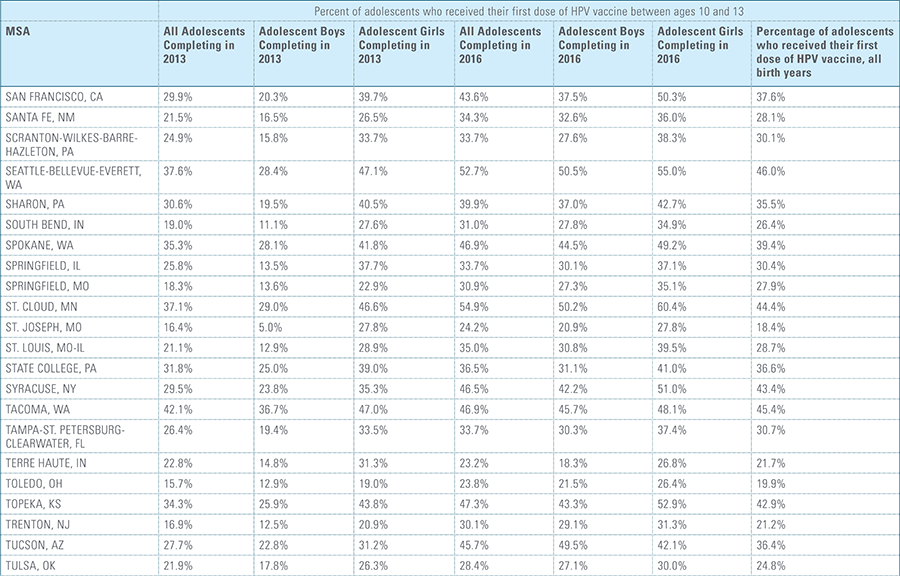
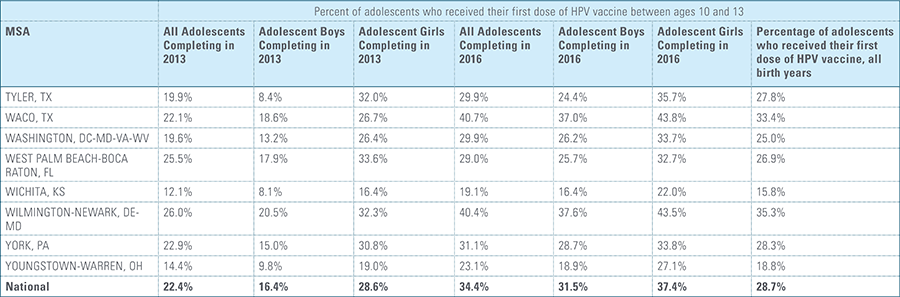
 In this report, the Blue Cross Blue Shield Association, in collaboration with HealthCore and Blue Health Intelligence (BHI), examines vaccination rates for U.S. commercially insured adolescents. The study focuses on three vaccines recommended by the Centers for Disease Control and Prevention (CDC) for adolescents: human papillomavirus (HPV), meningococcal and tetanus, diphtheria and pertussis (Tdap).1 It follows four birth cohorts of adolescents (born in 2000, 2001, 2002 and 2003) from ages 10 to 13 to determine whether they completed the recommended vaccine regimens “on time” by their 13th birthday (and thereby measures completion rates for the years 2013 through 2016).2
In this report, the Blue Cross Blue Shield Association, in collaboration with HealthCore and Blue Health Intelligence (BHI), examines vaccination rates for U.S. commercially insured adolescents. The study focuses on three vaccines recommended by the Centers for Disease Control and Prevention (CDC) for adolescents: human papillomavirus (HPV), meningococcal and tetanus, diphtheria and pertussis (Tdap).1 It follows four birth cohorts of adolescents (born in 2000, 2001, 2002 and 2003) from ages 10 to 13 to determine whether they completed the recommended vaccine regimens “on time” by their 13th birthday (and thereby measures completion rates for the years 2013 through 2016).2
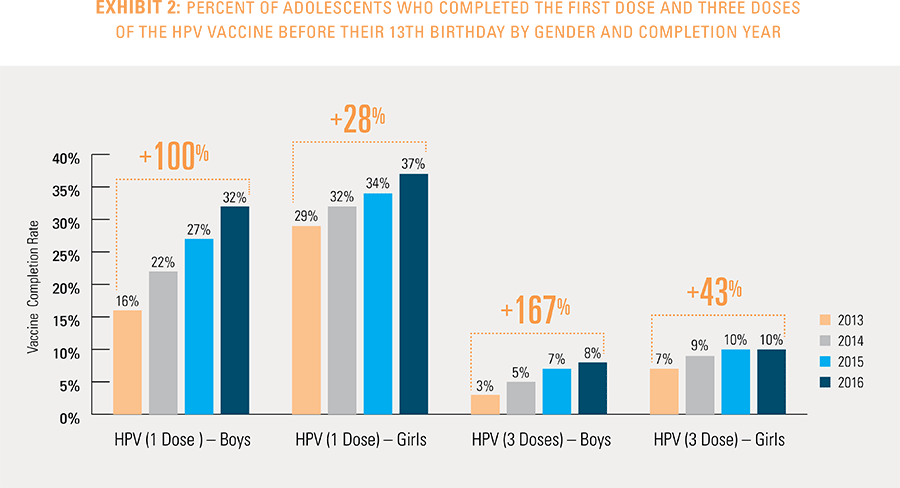
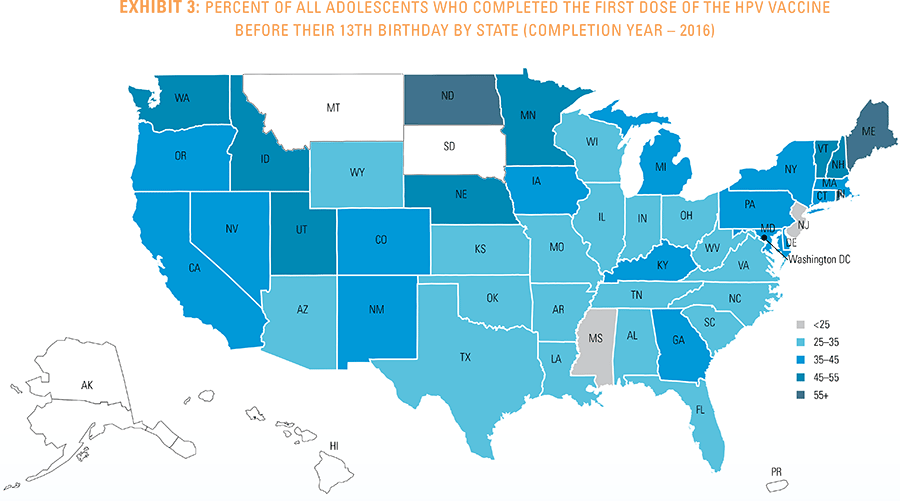
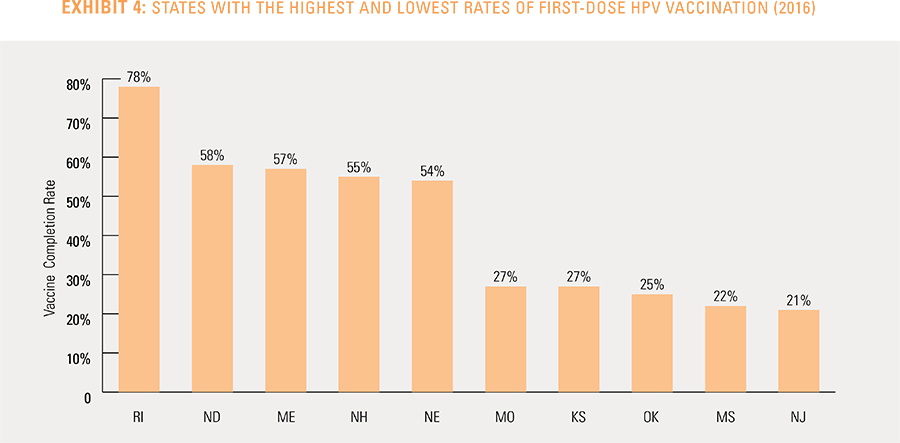
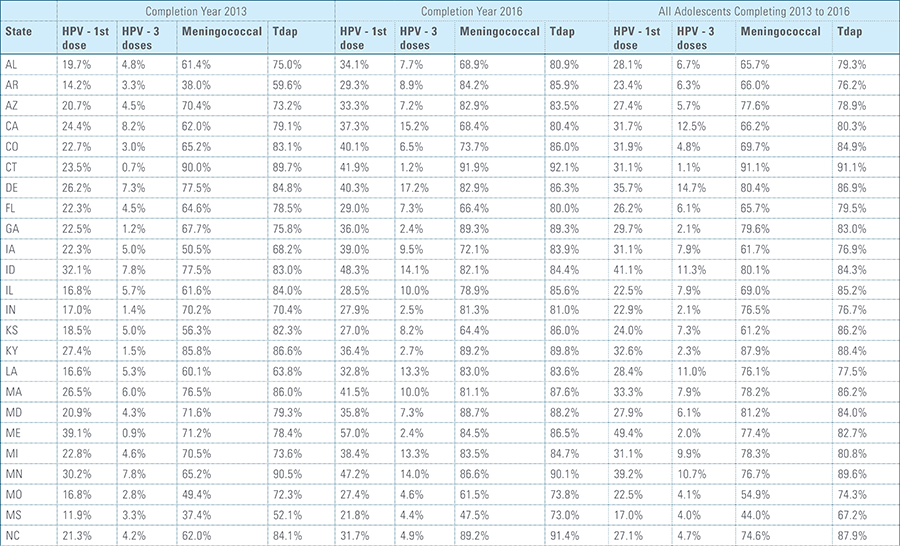
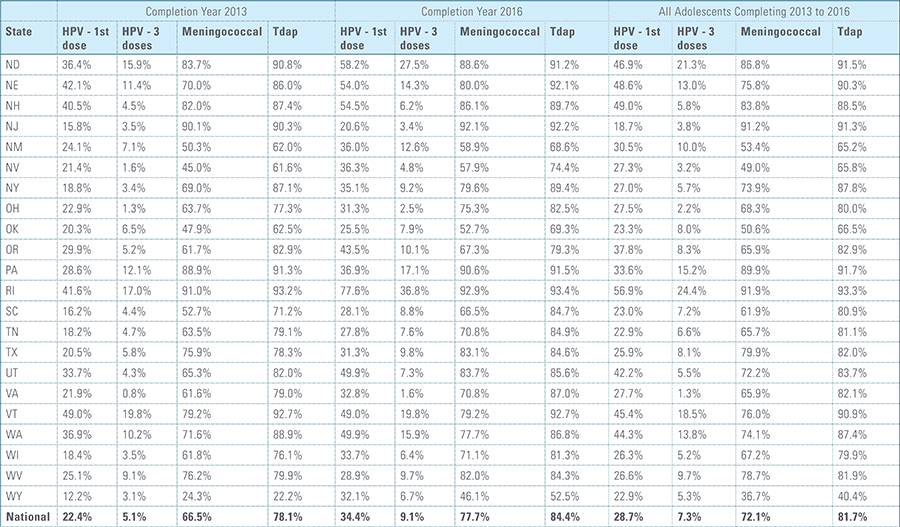
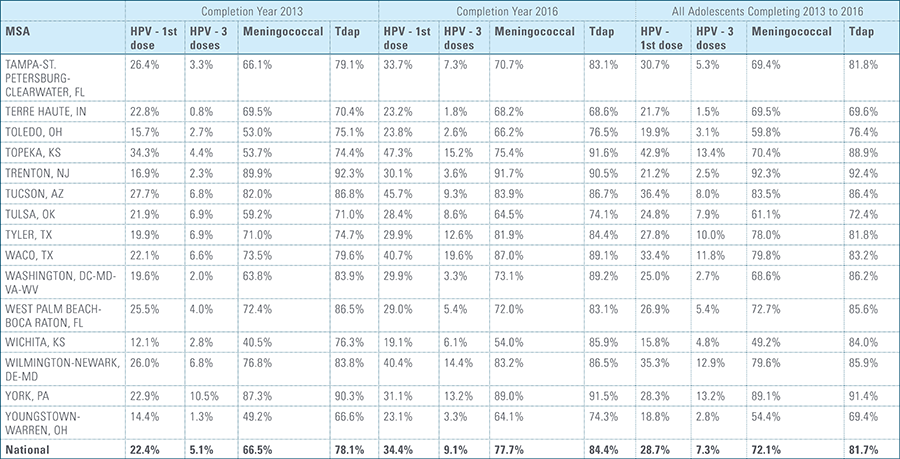
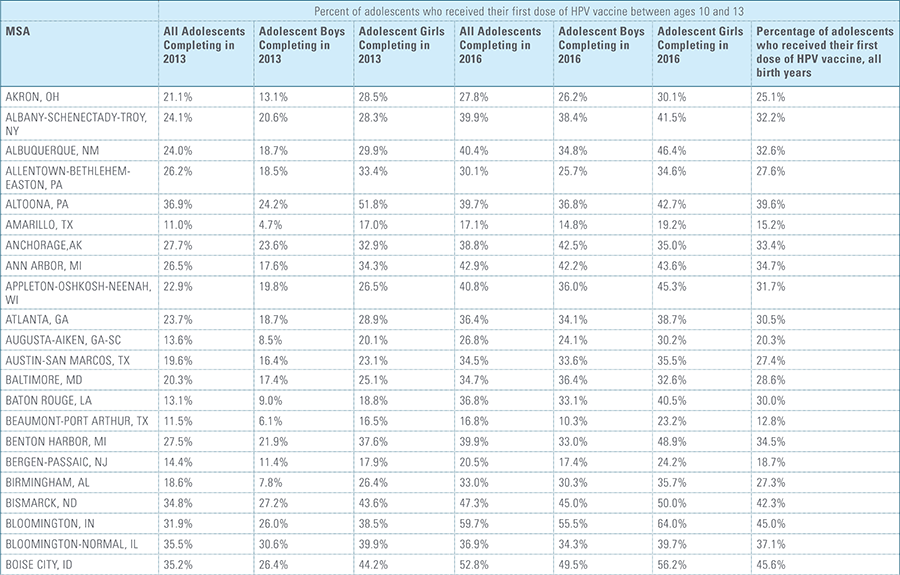
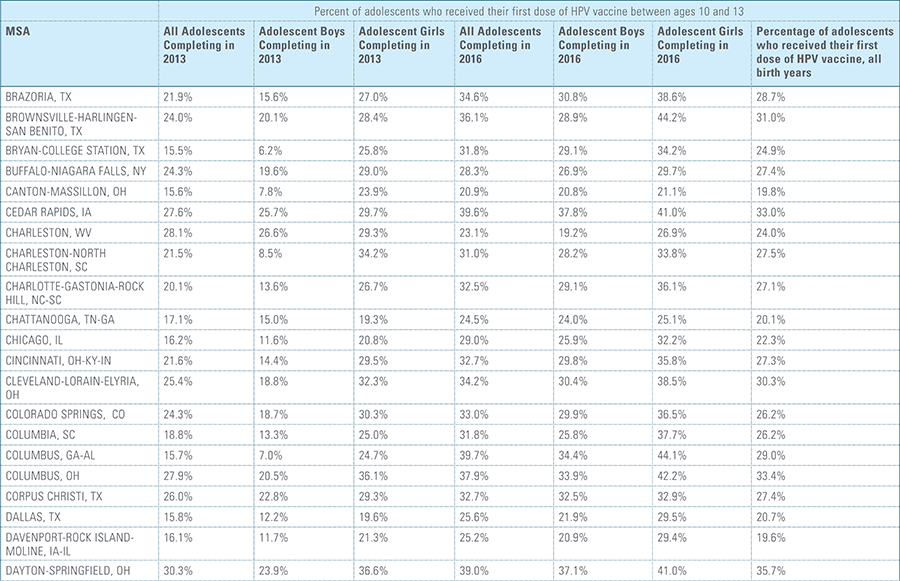
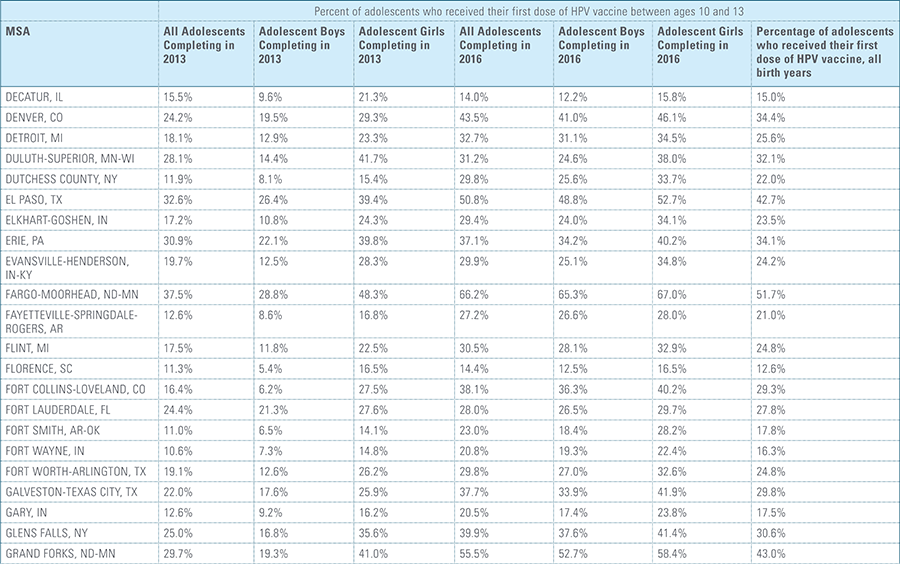
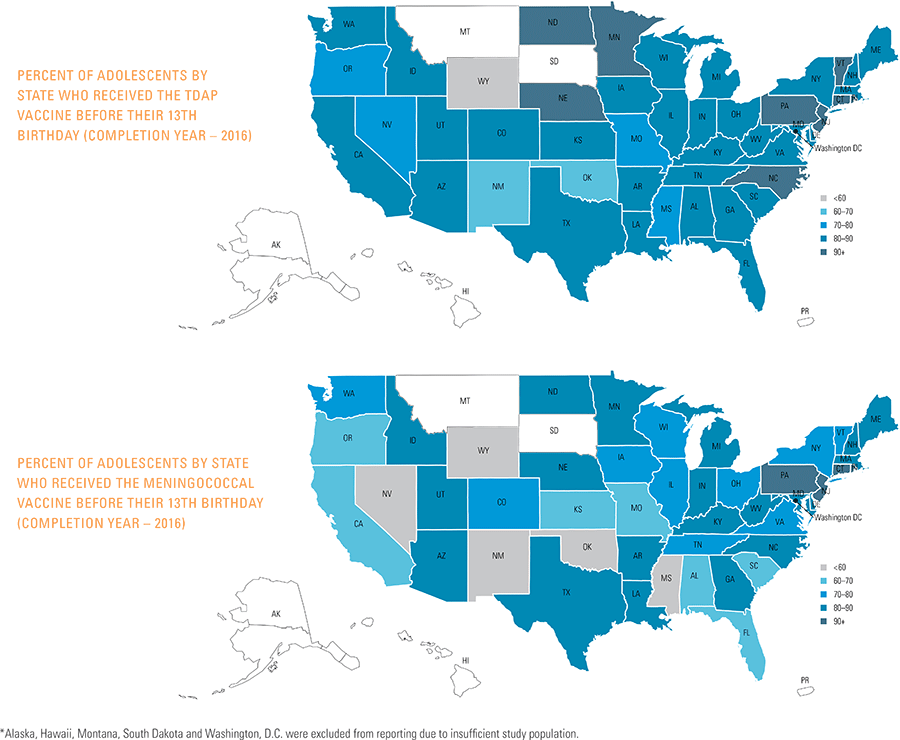
This study finds that national adolescent vaccination rates are fairly high for Tdap and meningococcal, but substantially lower for HPV. Wide geographic variation occurs in vaccination rates for all three vaccines throughout the country at both the state and local levels. Tdap and meningococcal vaccination rates are approximately equal for both boys and girls, while girls receive the HPV vaccine at higher rates than boys. Completion of the HPV vaccine regime for adolescents is a crucial step to protect against future infections, as the CDC estimates 31,500 deaths from cancers relating to the HPV virus occur each year.3



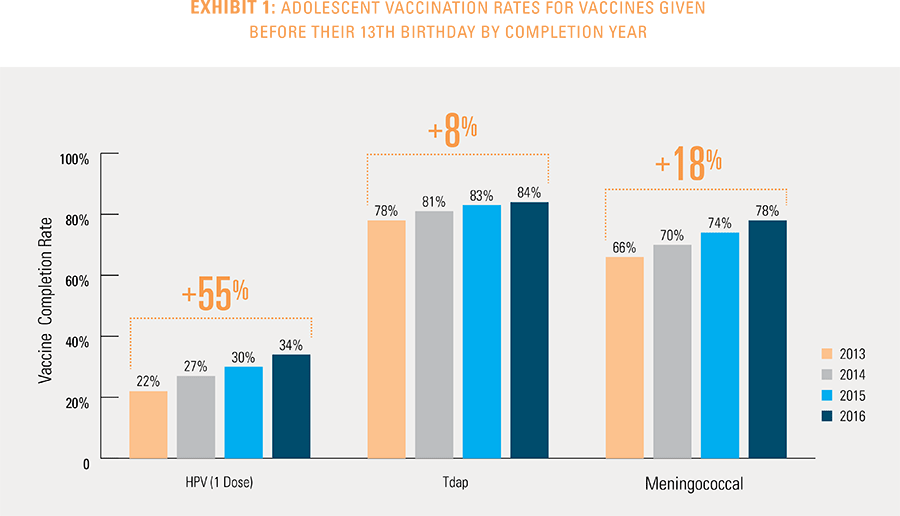
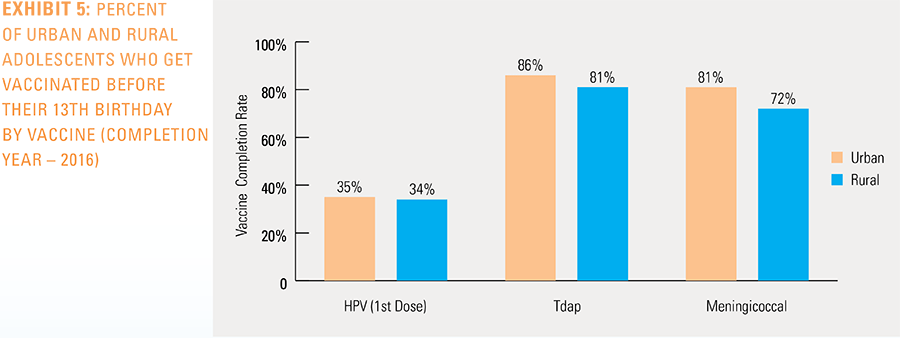
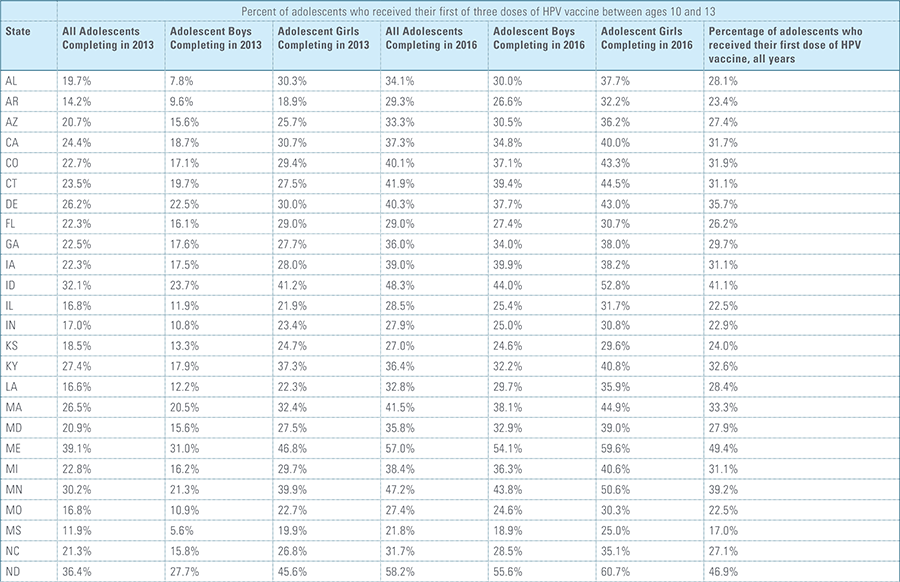
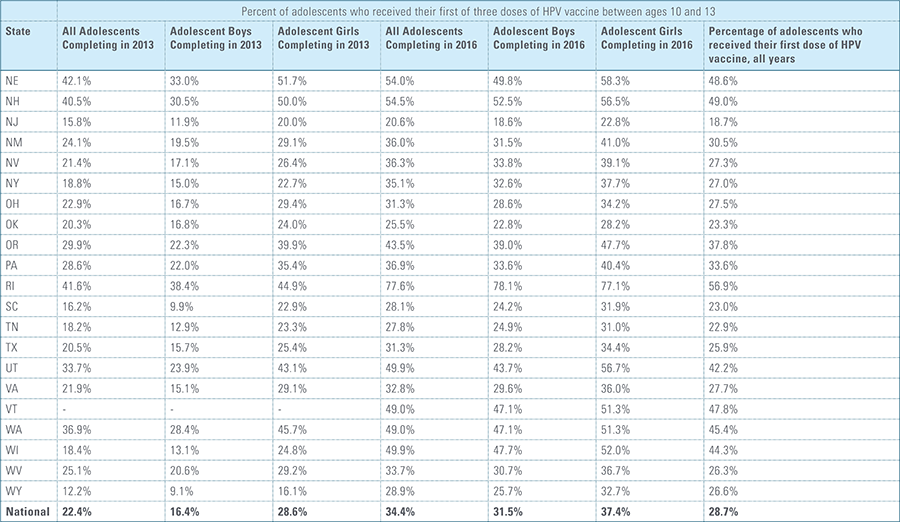
 Vaccination rates for the Tdap and meningococcal vaccines were nearly identical between boys and girls completing their vaccines in 2016.
Vaccination rates for the Tdap and meningococcal vaccines were nearly identical between boys and girls completing their vaccines in 2016.