Executive Summary
 Expansive news media coverage of football-related concussions and state legislation aimed at preventing participants of youth sports from “shaking off” signs of head injuries have coincided with a spike in the number of concussion diagnoses, according to Blue Cross and Blue Shield (BCBS) companies’ medical claims data.
Expansive news media coverage of football-related concussions and state legislation aimed at preventing participants of youth sports from “shaking off” signs of head injuries have coincided with a spike in the number of concussion diagnoses, according to Blue Cross and Blue Shield (BCBS) companies’ medical claims data.
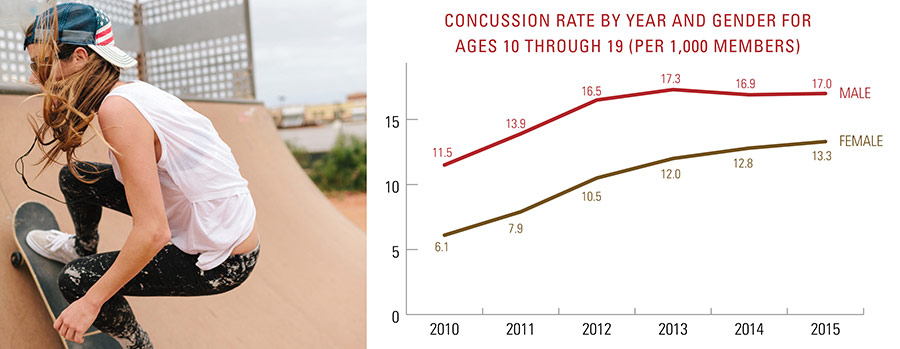
Concussion diagnoses increased 43 percent from 2010 through 2015 in the U.S. Additionally, concussion diagnoses spiked 71 percent for patients ages 10 through 19 during the same time span. For this age group, the fall is peak concussion season, during which time a dramatic spike in diagnoses occurs for males. Concussion diagnoses for young males in the fall are nearly double that of young females. Even though concussion diagnoses for adults ages 20 through 64 increased 26 percent over the same time period, there was little seasonal change compared to their younger counterparts.
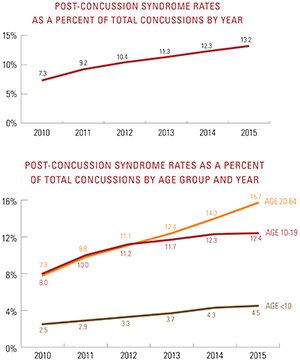
The percentage of concussion patients across all ages diagnosed with post-concussion syndrome nearly doubled between 2010 and 2015. Throughout the study, post-concussion syndrome was diagnosed equally for both males and females ages 10 through 19 who suffered concussions. Females ages 20 through 64 who suffered concussions, however, were nearly 60 percent more likely to receive such a diagnosis than males.
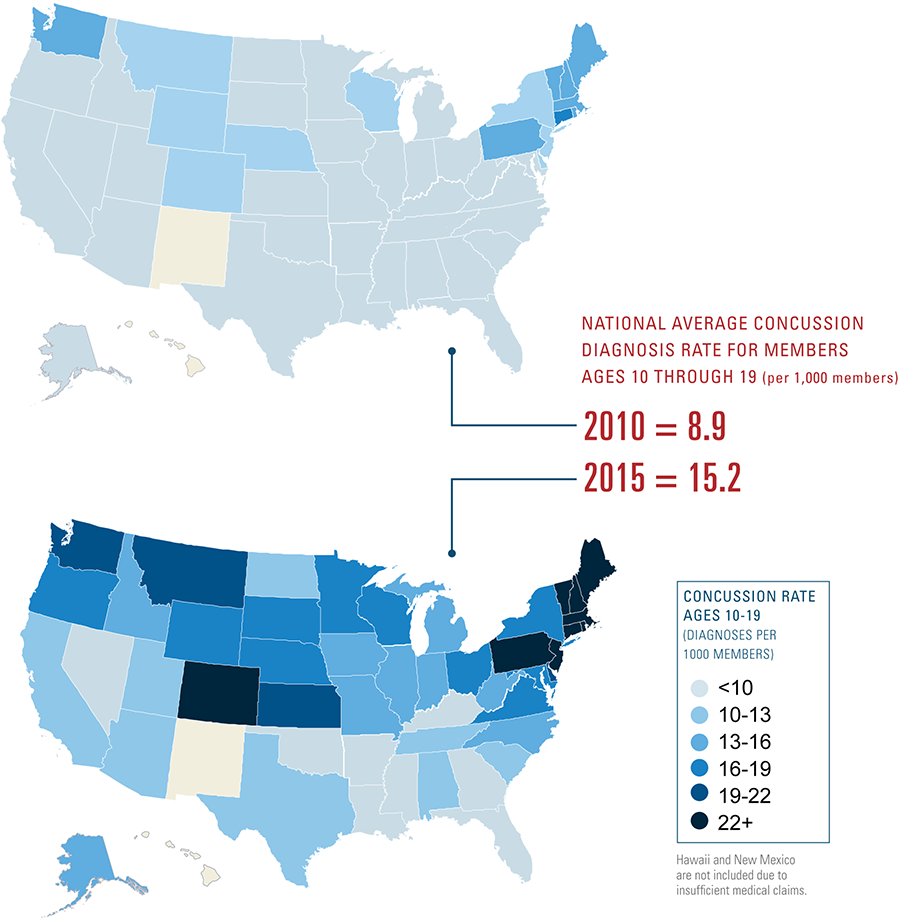
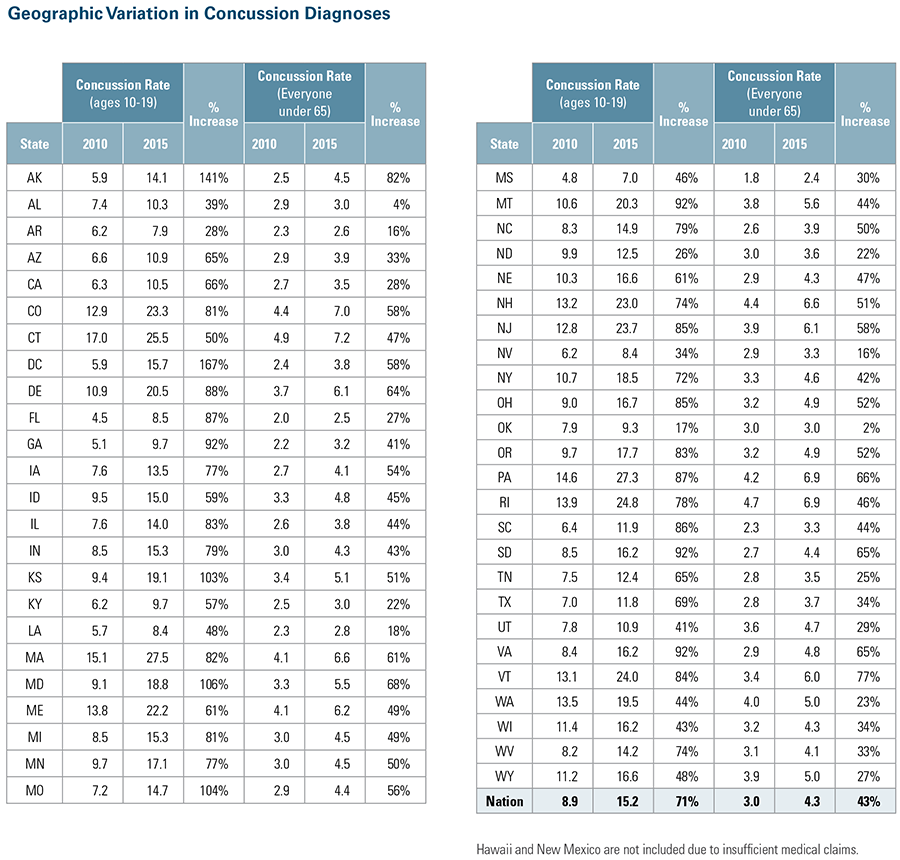
Finally, BCBS data in 2015 show that patients ages 10 through 19 in some states have nearly a three times higher rate of concussions diagnosed than in other states. The intent of this report is to document concussion diagnosis rates and increase awareness that could help inform policy and concussion treatment practices for school districts and medical professionals.


 News reports on the long-term effects of concussions and chronic traumatic encephalopathy (
News reports on the long-term effects of concussions and chronic traumatic encephalopathy (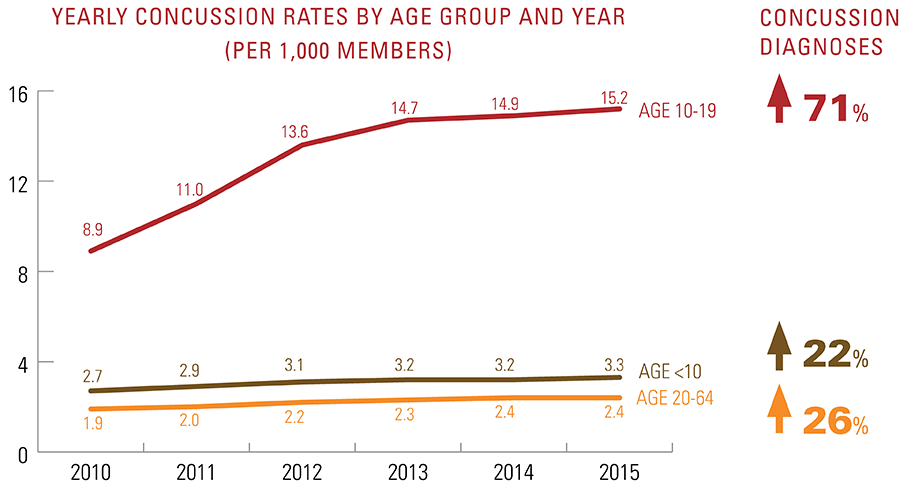
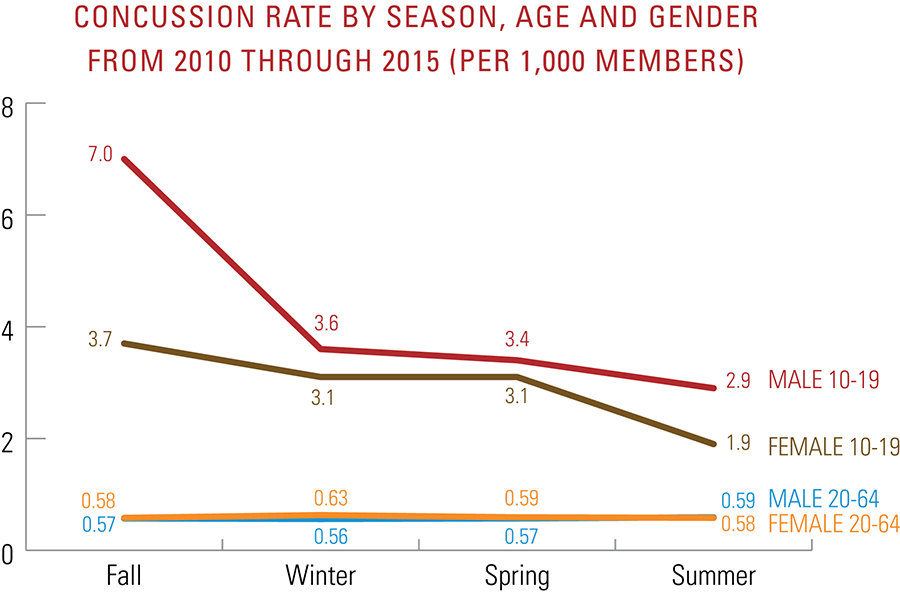
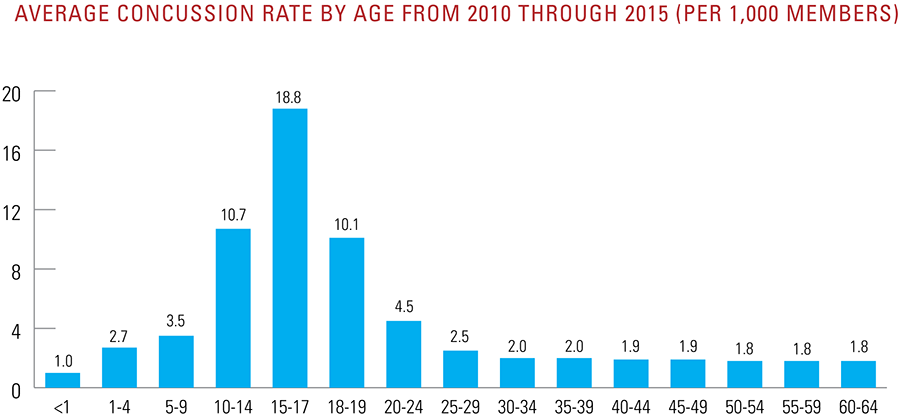
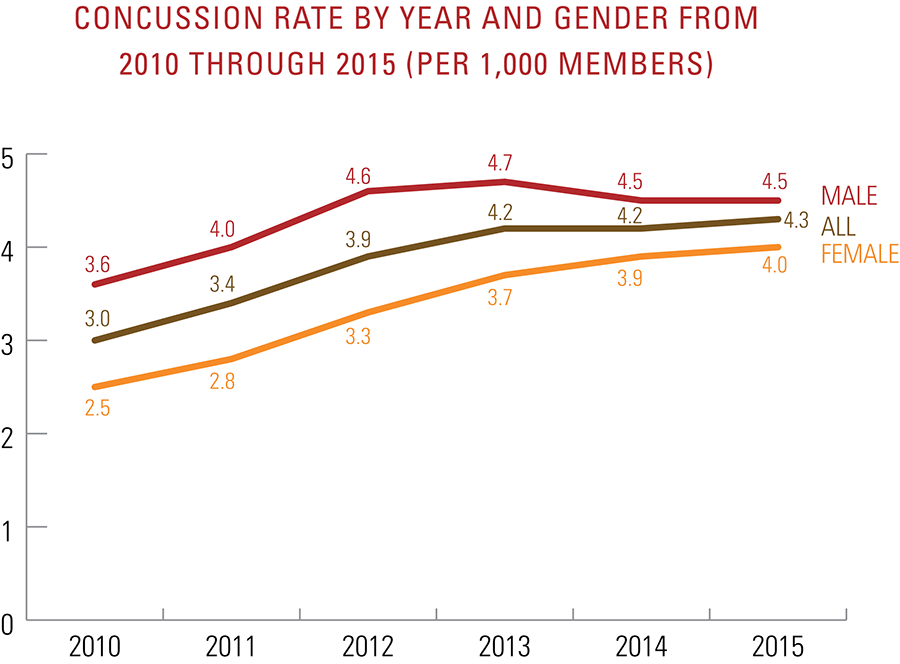
 Data show that patients ages 10 through 19 are over five times more likely to be diagnosed with a concussion than all other age groups combined, with young males being diagnosed 49 percent more than young females. In the fall, there is a dramatic spike in concussion diagnoses, with young males being diagnosed at a rate of 7.0 per 1,000 members, which is nearly double that of young females at 3.7 per 1,000 members. Fall is when the most popular contact sports are in session (e.g. football and, in most states, soccer) at schools and parks. There are no significant seasonal differences for adults ages 20 to 64.
Data show that patients ages 10 through 19 are over five times more likely to be diagnosed with a concussion than all other age groups combined, with young males being diagnosed 49 percent more than young females. In the fall, there is a dramatic spike in concussion diagnoses, with young males being diagnosed at a rate of 7.0 per 1,000 members, which is nearly double that of young females at 3.7 per 1,000 members. Fall is when the most popular contact sports are in session (e.g. football and, in most states, soccer) at schools and parks. There are no significant seasonal differences for adults ages 20 to 64.