Study suggests AI is boosting hospital billing
An unusual trend is emerging in medical records of new mothers: The records list severe blood loss during childbirth, even though the patient never received a transfusion. Hospital systems and artificial intelligence companies are frequently announcing new efforts to use AI to document and bill for patient visits. This kind of automation can streamline workflows around coding, the process of translating health care services into standardized codes to use for billing and insurance.
But a new analysis suggests the use of the technology may be causing a mismatch between the care patients receive and the bills hospitals send to insurance companies. When coding and care aren’t aligned, costs rise for everyone.
For the analysis, the data analytics team from Blue Health Intelligence® (BHI®) looked at de-identified claims data from tens of thousands of maternity admissions. At some hospitals, there was a significant increase in cases coded for acute posthemorrhagic anemia, a serious condition that typically signals severe blood loss and a need for extra medical attention and treatment, like a blood transfusion.
The data analyzed by BHI showed many patients flagged with this diagnosis never received blood transfusions. This gap raises important questions about how diagnoses are documented and why accuracy matters.
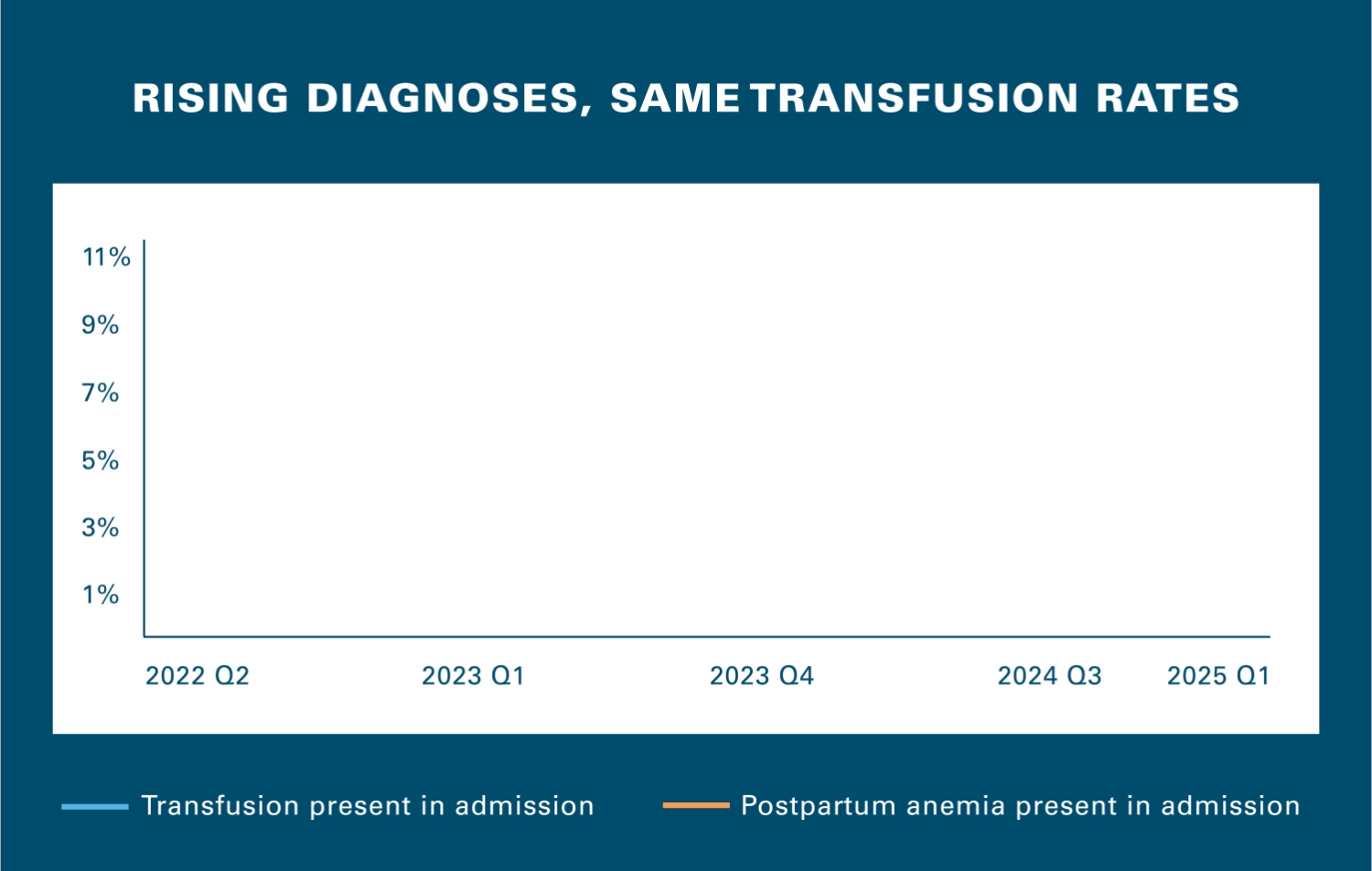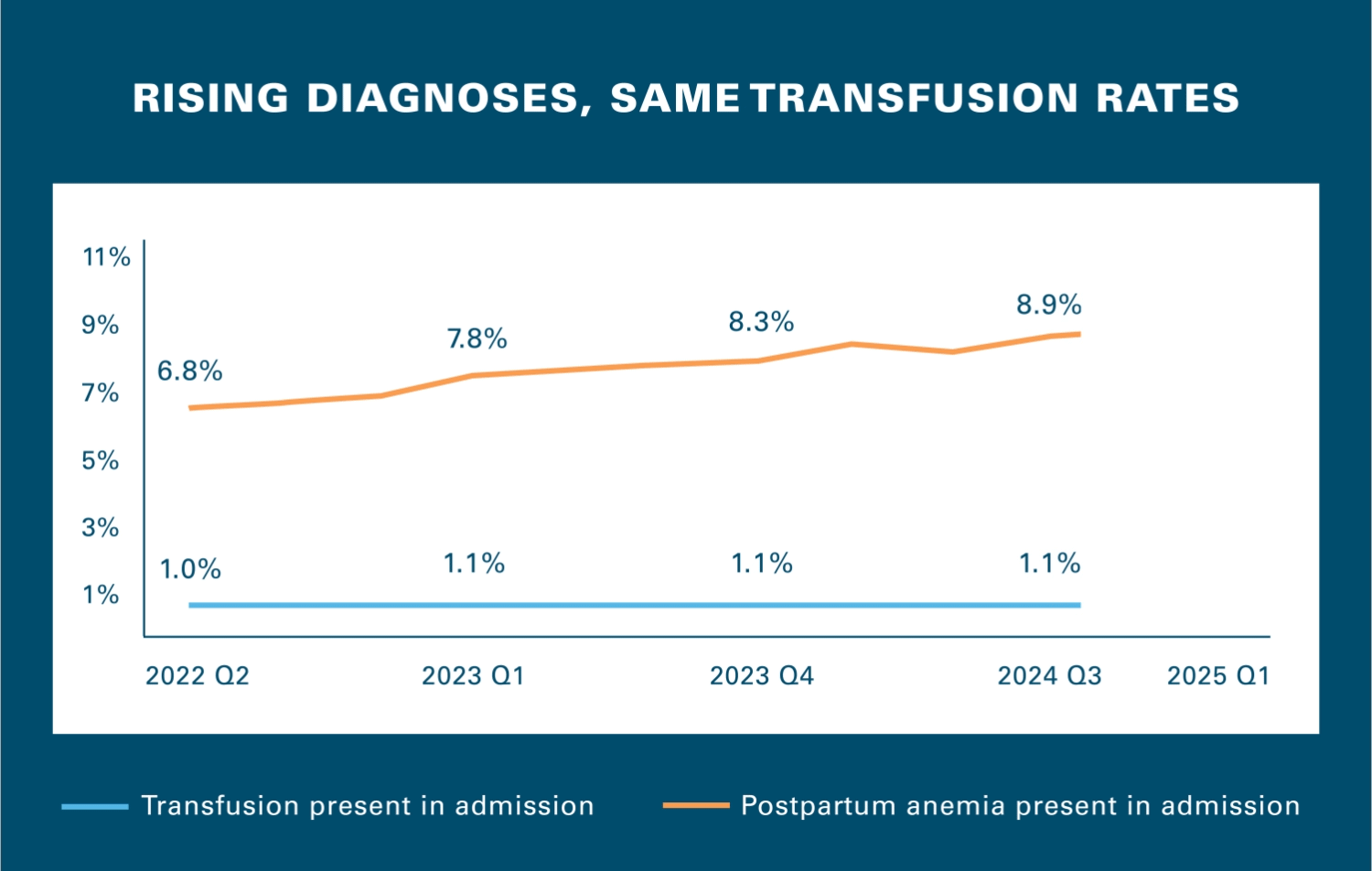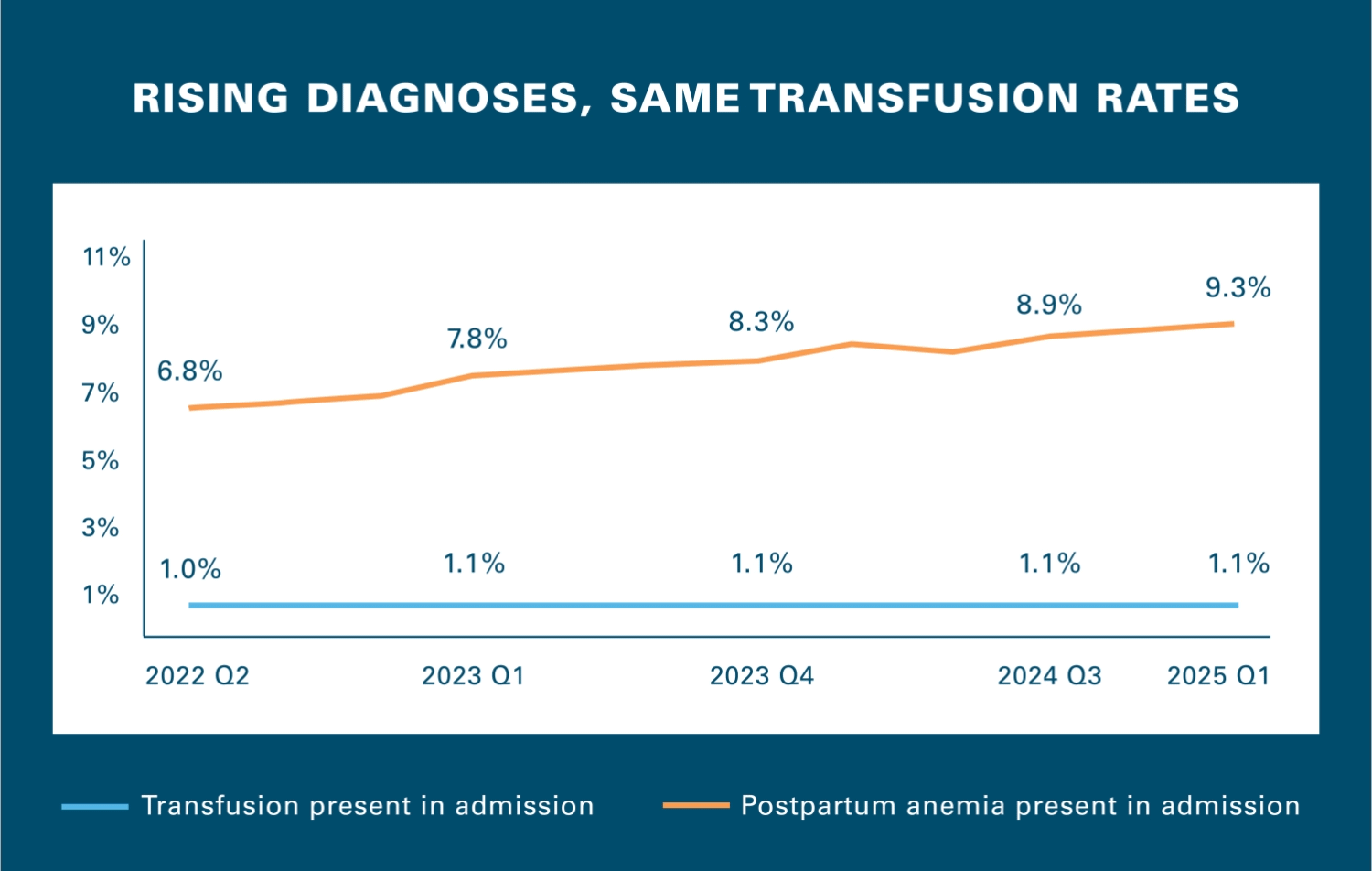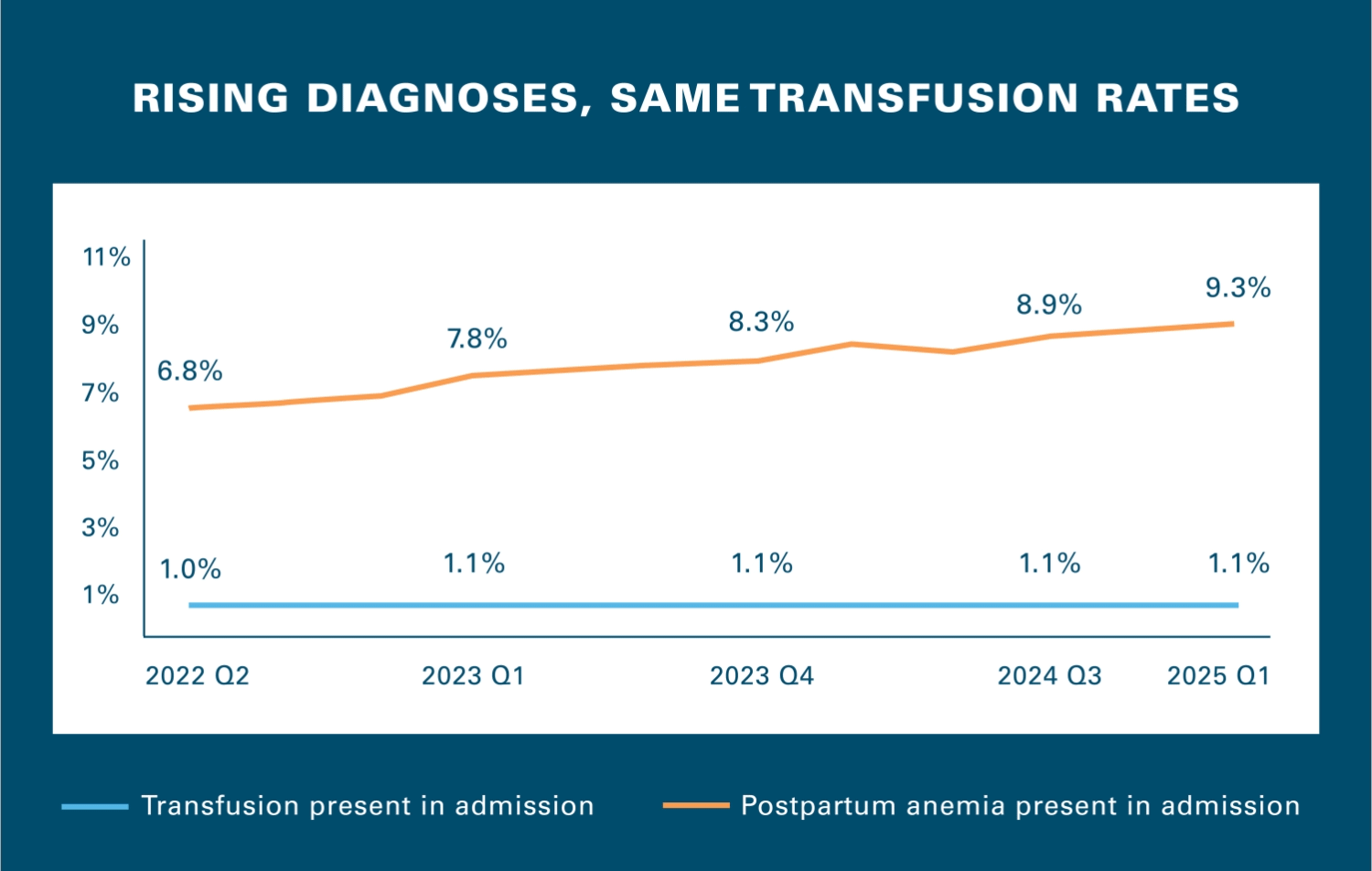
“Something is disconnected,” said Dr. Razia Hashmi, VP of Clinical Affairs at the Blue Cross Blue Shield Association (BCBSA).
“Among hospitals showing the fastest rise in diagnoses of post-partum anemia, the rise in patients coded with this condition wasn’t paired with the level of care we would have expected, and the patterns we’re seeing point to AI‑enabled coding. These hospitals also had a far higher rate of this hemorrhaging when compared with similar health systems in the same region," said Dr. Hashmi.
With the team at BHI, BCBSA reviewed hospitals where either the hospital or a vendor had publicly disclosed its use of AI. Among other features, these AI-enabled clinical documentation and coding technologies reportedly leverage ambient listening to capture clinical interactions and analyze lab reports and physician notes to automatically assign billing codes. Researchers often saw sharp spikes in the number of patients coded with complex conditions at these high-growth facilities; far more complex than the care delivered in the acute posthemorrhagic anemia case study, a practice known as upcoding.
Upcoding is a real contributor to our country’s affordability crisis, where all of us pay for care at levels that were never delivered. This research suggests AI is making it worse.
The BHI analysis found that the increase of acute posthemorrhagic anemia alone at the analyzed hospitals added $22 million to maternity admission costs in one year.
The price tag of AI upcoding
Coding for conditions without treating those conditions means hospitals may be paid for care that was not delivered, which inflates premium costs for everyone. The BHI analysis found that in 2024, Blue Cross and Blue Shield (BCBS) companies saw a sharp rise in what they paid facilities for complex conditions. For example, a patient admitted for a stroke may also be listed in patient records as having kidney disease. Each secondary diagnosis allows the hospital to bill insurance companies more. Costs are artificially increased, however, when secondary diagnoses are added without evidence of treatment.
We looked at all facilities nationwide and saw that some hospitals followed the same patterns we see in known AI adopters. Those hospitals had some of the biggest jumps in complexity and payments. One facility’s complexity rating increased 6.7% after announcing its switch to AI, compared to just 0.9% among other facilities in the same state.
Here’s what that looks like in dollars:
About $663 million in inpatient spending
may be tied to AI-powered coding tools
At least $1.67 billion in outpatient spending
may be linked to more aggressive coding practices
And adoption is widespread. Nearly half (46%) of hospitals and health systems use AI in billing, coding and claims, according to a 2023 Healthcare Financial Management Association (HFMA) and AKASA survey. Recent federal data shows the trend is accelerating: 7 in 10 U.S. hospitals used predictive AI in 2024, and AI use for billing jumped 25 percentage points year over year.
As AI moves from experimental to essential in clinical settings, its use in coding and billing is likely to grow, raising the stakes for accuracy.
What can be done?
When used carefully, this technology can help ease physician burnout by reducing paperwork, letting them focus more on patient care and less on forms. We need to analyze our collective data to better spot trends where AI is not accurate and share learnings so we can manage appropriate care effectively. BCBSA and BCBS companies are addressing this issue at a national and local level to drive better outcomes for patients — working with our provider partners to better align payment with the accurate representation of appropriately delivered care.
To tackle AI-driven upcoding, we’re focused on supporting BCBS companies with:
- Using data to spot upcoding trends
- Establishing clear expectations for hospitals using AI coding tools to ensure billing matches delivered care
Harnessing data and working together, we can make sure every dollar spent reflects appropriate care delivered.
Blue Health Intelligence (BHI)
Blue Health Intelligence (BHI) is a trade name of Health Intelligence Company LLC, an independent licensee of the Blue Cross Blue Shield Association. The trademarks included in this document are owned by each respective company, used for informational purposes only, and do indicate any endorsement or affiliation.
The latest in healthcare, delivered.
Subscribe to stay in the know on health care industry news and insights.