Executive Summary
 In this report,1 Blue Cross Blue Shield Association examines diagnosed major depressive disorder (major depression) using the breadth and depth of data available through the Blue Cross Blue Shield Health Index.SM According to the BCBS Health Index, major depression is the second most impactful condition on overall health for commercially insured Americans, second to hypertension (high blood pressure).
In this report,1 Blue Cross Blue Shield Association examines diagnosed major depressive disorder (major depression) using the breadth and depth of data available through the Blue Cross Blue Shield Health Index.SM According to the BCBS Health Index, major depression is the second most impactful condition on overall health for commercially insured Americans, second to hypertension (high blood pressure).
Major depression is a complex condition that has a substantial impact on overall health and wellness. It is crucial to effectively address and manage this condition to improve the health of all Americans.

Specific Findings
- Major depression has a diagnosis rate of 4.4 percent in the United States, affecting more than 9 million commercially insured Americans.
- Diagnoses of major depression have risen dramatically by 33 percent since 2013. This rate is rising even faster among millennials (up 47 percent) and adolescents (up 47 percent for boys and 65 percent for girls).
- Women are diagnosed with major depression at higher rates than men (6 percent and nearly 3 percent, respectively).
- People diagnosed with major depression are nearly 30 percent less healthy on average than those not diagnosed with major depression. This decrease in overall health translates to nearly 10 years of healthy life lost for both men and women.4
- A key reason for the lower overall health of those diagnosed with major depression is that they are likely to also suffer from other health conditions. Eighty-five percent of people who are diagnosed with major depression also have one or more additional serious chronic health conditions and nearly 30 percent have four or more other conditions.5
- People diagnosed with major depression use healthcare services more than other commercially insured Americans. This results in more than two times higher overall healthcare spending ($10,673 compared to $4,283).

The Impact of Major Depression on Overall Health
Major depression is the second most impactful condition on the overall health of commercially insured Americans, as measured by the BCBS Health Index. Only hypertension, with a nearly five-fold higher diagnosis rate, has a broader health impact on Americans.
The overall health of people diagnosed with major depression as measured by the BCBS Health Index is 27 percent lower than for those without this diagnosis, due to diagnoses of both major depression and one or more additional health conditions (see Exhibit 1)6. This difference in overall health, on average, translates to a reduction in future healthy life expectancy of 9.5 years for women and 9.7 years for men. This reduction in future healthy life expectancy is due not only to major depression but also to the increased likelihood of being diagnosed with other conditions that often coincide with a major depression diagnosis.7
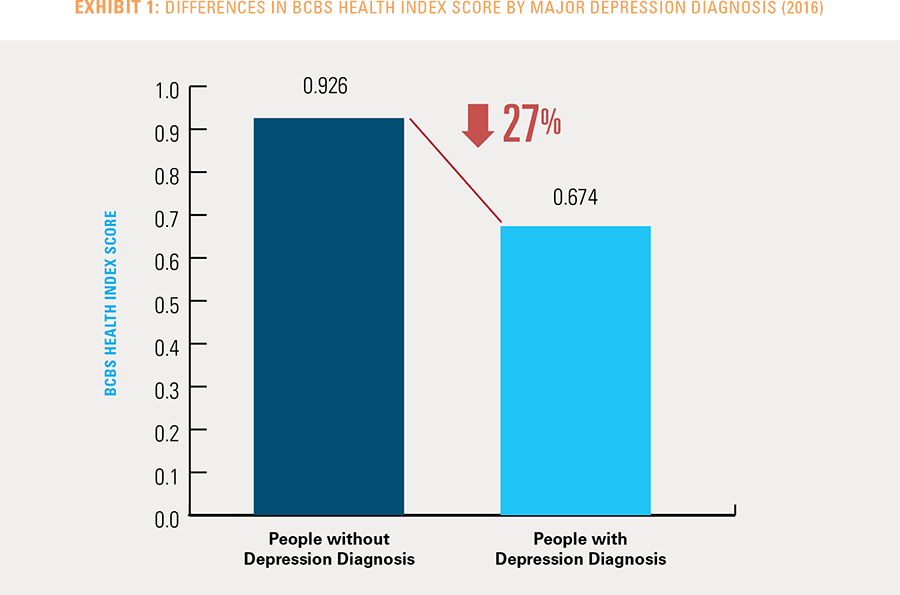
The Diagnosis of Major Depression
Major depression impacts the lives of 4.4 percent of commercially insured Americans, or roughly 9 million people. This diagnosis rate has increased steadily since 2013 across all gender and age groups.
Women are more than twice as likely as men to be diagnosed with major depression (6 percent compared to 2.8 percent, respectively), though diagnosis rates for each group rose by 33 percent since 2013 (see Exhibit 2).
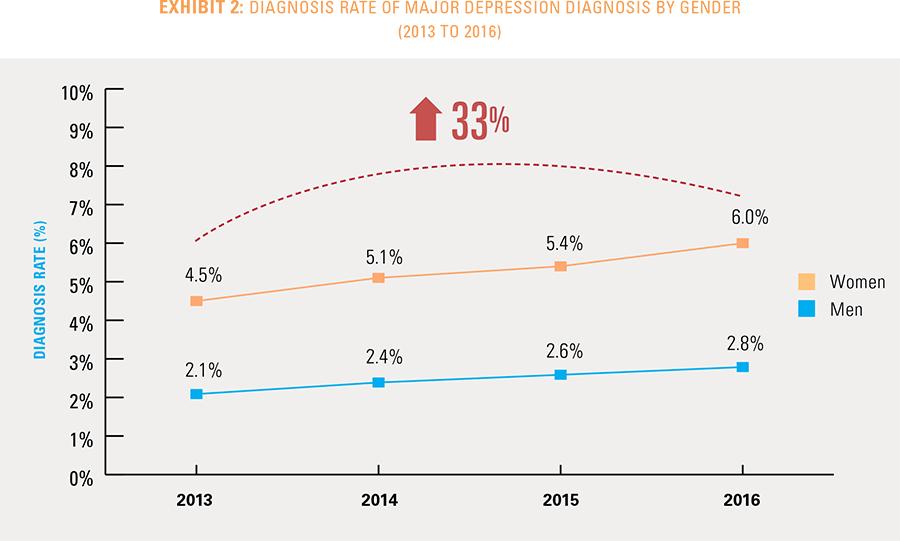
Americans diagnosed with major depression can also be divided into four age groups: adolescents (ages 12 to 17), millennials (ages 18 to 34), adults (ages 35 to 49) and mature adults (ages 50 to 64).
Major depression diagnosis rates are steadily increasing across all age groupings. The most dramatic rise in major depression diagnosis is among those under 35 years of age. Between 2013 and 2016 diagnoses increased 63 percent among adolescents and 47 percent among millennials (see Exhibit 3). Gender differences among millennials were similar but among adolescents there was a 65 percent increase for girls compared to a 47 percent rise for boys. These quickly rising rates of diagnosed major depression in younger age groups can have broader implications on future healthcare needs as they grow into later adulthood. Effective diagnosis and management of major depression in these early years is crucial to positively impact future health and wellness.
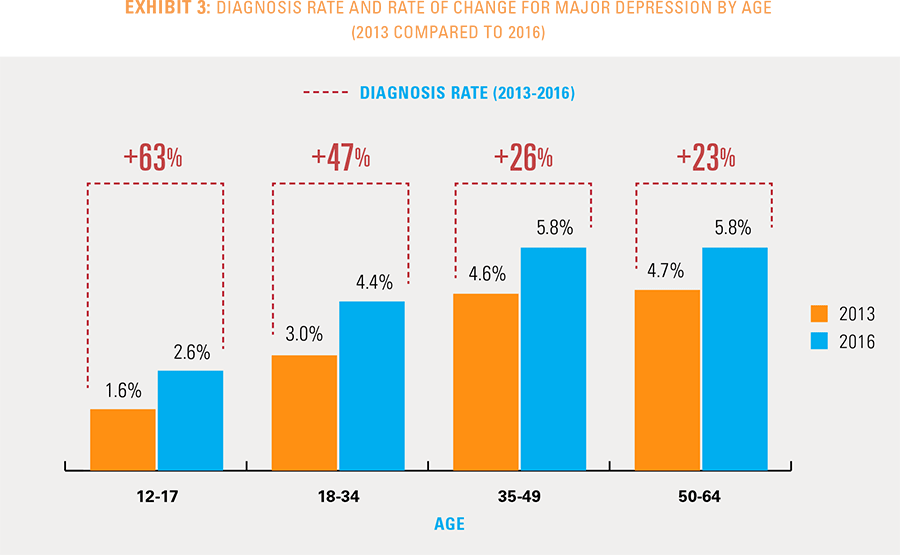
Geographic Variation of Major Depression
Wide geographic variation exists in the diagnosis of major depression among people in each state. Differences in the effort to screen for major depression can produce varying diagnoses rates for this condition across states. There are higher rates of major depression in New England, the Pacific Northwest and various pockets throughout the South and Midwest. Rhode Island has the highest major depression diagnosis rate at about 6 percent, while Hawaii shows the lowest rate at about 2 percent. Nonetheless, 49 of the 50 states had rising diagnosis rates of major depression from 2013 to 2016, with only Hawaii
showing a slight decline (see Exhibit 4). (See Appendices B and C for more detailed information by state and metropolitan statistical area, or MSA.)
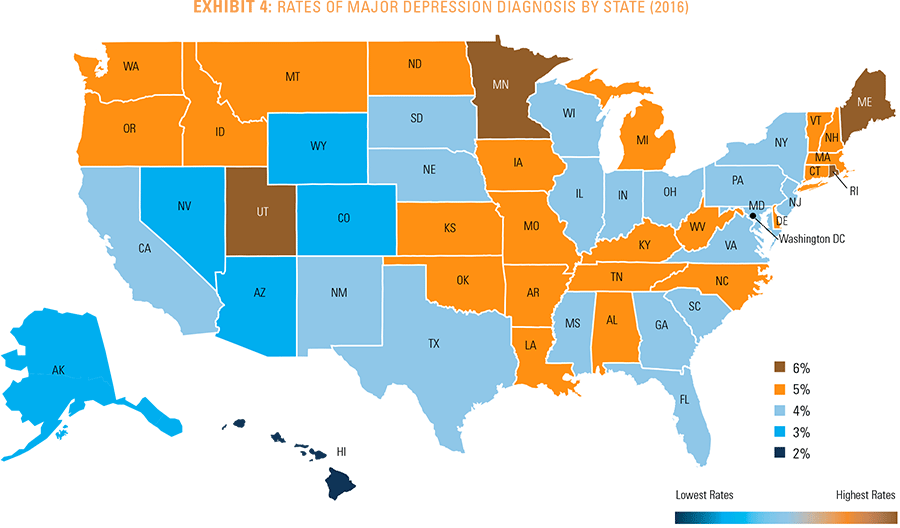
The Link Between Major Depression and Other Health Conditions
Americans diagnosed with major depression often suffer from a number of additional chronic, behavioral health and pain-related health conditions.8 However, it should be noted that claims-based data cannot determine when major depression precedes or follows other serious health conditions nor to what degree major depression may cause (or be caused by) these other health conditions.
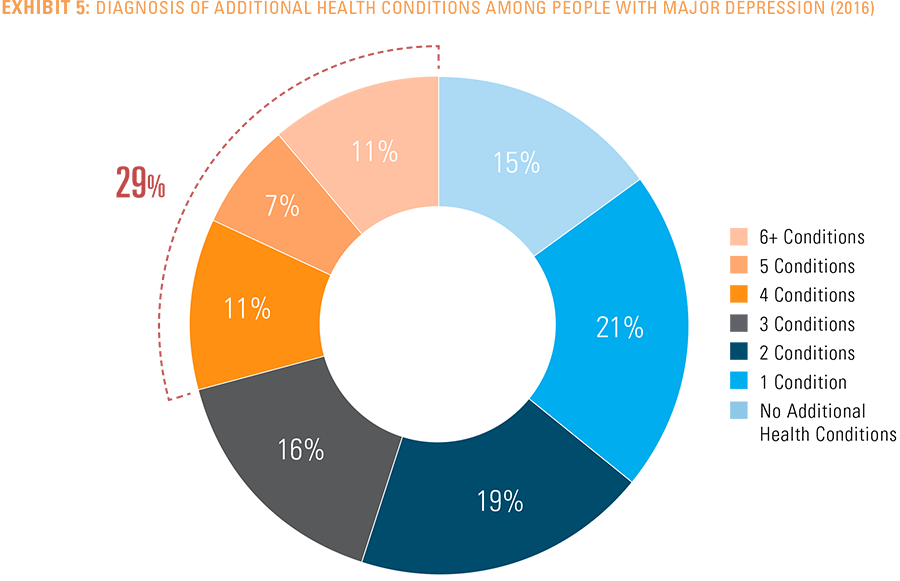
Of the more than 9 million people diagnosed with major depression in 2016, only 15 percent were diagnosed with that condition alone. Eighty-five percent were diagnosed with both major depression and one or more additional health condition.9 Twenty-one percent of people had one additional health condition, 19 percent had two additional health conditions and 29 percent had four or more additional health conditions (see Exhibit 5).
Further exploring the relationship between major depression and other common health conditions reveals that people diagnosed with major depression are twice as likely to also suffer from one or more other chronic diseases, three times as likely to suffer from pain-related disorders and injuries, and seven times as likely to suffer from alcohol or substance use disorders than people who do not have major depression.10
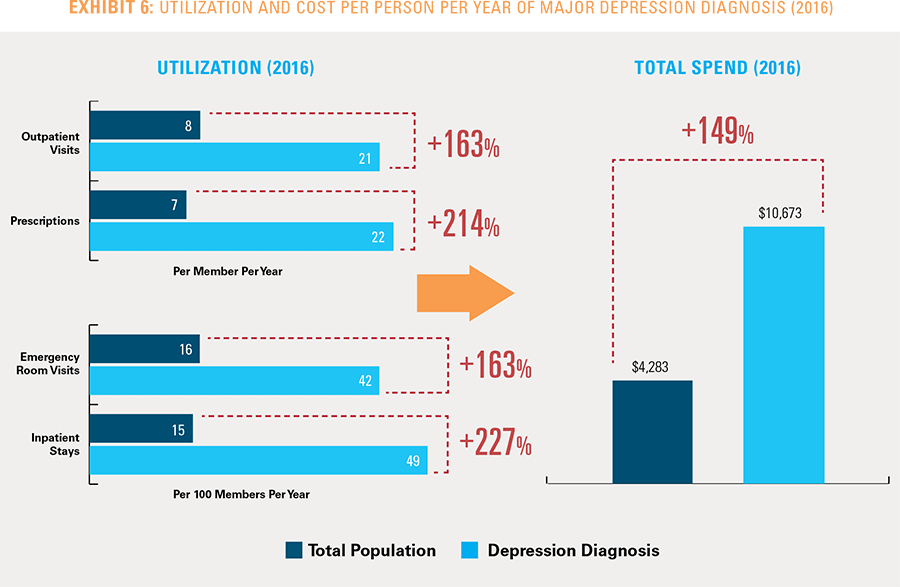
Americans often utilize several healthcare services to manage their health needs. When comparing those who do have a major depression diagnosis to those without in 2016, people with major depression have significantly higher utilization rates of healthcare services. This increased utilization links to more than two-fold higher average healthcare costs for those with major depression at $10,673 compared to $4,283 for others spending on healthcare services (see Exhibit 6).11 The average amount spent per person per year to treat only major depression is $920. However, healthcare spending on major depression can vary widely from person to person.12
Conclusion
Major depression is a health condition affecting more than 9 million commercially insured Americans. Major depression diagnosis is growing quickly, especially for adolescents and millennials. This health condition has many implications for the future healthcare needs for these younger Americans. Higher rates of major depression can translate to increased utilization of healthcare services, leading to more than twice the amount of healthcare costs than for those without depression. Further, wide geographic variation exists in the diagnosis of major depression across the U.S.
While major depression is the second most impactful health condition for the nation, it is complicated by an increased likelihood of overlapping diagnoses of other chronic, behavioral health and pain-related conditions. Further education and research are needed to identify methods for physicians to effectively treat major depression and for patients to begin a path to recovery and better overall health.
Appendix A: THE BCBS Health IndexSM
The BCBS Health Index is a unique health metric that provides a better understanding about which diseases and conditions most impact Americans’ overall quality of life. The BCBS Health Index identifies more than 200 health conditions and quantifies how each condition affects Americans’ health, life expectancy and well-being.
Powered by data from more than 41 million BCBS commercially insured members per year from birth to age 64, this extensive resource brings an unmatched contribution to other available health data to support national and local discussions about how to improve healthcare in the U.S. Focusing on claims and other healthcare data as opposed to aggregated government statistics, the BCBS Health Index provides a unique view of America’s health down to the county level.
The BCBS Health Index is part of Blue Cross and Blue Shield companies’ commitment to improving the health of all Americans by uniting policymakers, community leaders, healthcare professionals and business leaders around data-driven insights to spark real change across the nation.
This is the twentieth study of the Blue Cross Blue Shield, The Health of America Report series. For more information and to read past reports, visit www.bcbs.com/the-health-of-america.
METHODOLOGY: HOW THE BCBS HEALTH INDEX WORKS
The BCBS Health Index assigns defined populations in the United States a health index score between 0 and 1, where 1 represents optimal health and anything less than 1 represents the adverse impact of illness or disease on longevity and quality of life. For example, a health index score of 0.9 indicates that, on average, that population is living at 90 percent of its optimal health. In other words, the population could increase (to some level up to 10 percent) its average healthy lifespan by addressing the health conditions most impacting their local communities.
The BCBS Health Index score is calculated by using blinded claims data from more than 41 million commercially insured BCBS members annually and determining which condition a person has by mapping ICD-9 diagnoses codes to more than 200 health condition categories. The health impact of each condition on a person’s health is based on the estimated years lost due to the risk of premature death and the disabling effects of the condition. For each individual, these years of life lost are subtracted from the person’s optimum life expectancy (as determined by the person’s age and gender using actuarial life tables) to calculate an estimated life expectancy. This estimated life expectancy is then divided by the optimum life expectancy to get an estimate of health between 0 and 1 where “1” means the individual is living at their optimal health due to having no health conditions and a number less than 1 is a proportion of this optimal health. These individual-level estimates are then aggregated to create an overall “health score” for the population of interest.
The formal calculation is:
BCBS Health Index = [Optimum Life Expectancy – (Mortality + Disability)] / Optimum Life Expectancy
Where “optimum life expectancy” is derived from an actuarial life table, “mortality” is years of life lost due to risk of premature death as determined by the Center for Disease Control (CDC), and “disability” is years of living with a disability based on the Institute for Health Metrics and Evaluation’s (IHME) disability weights.
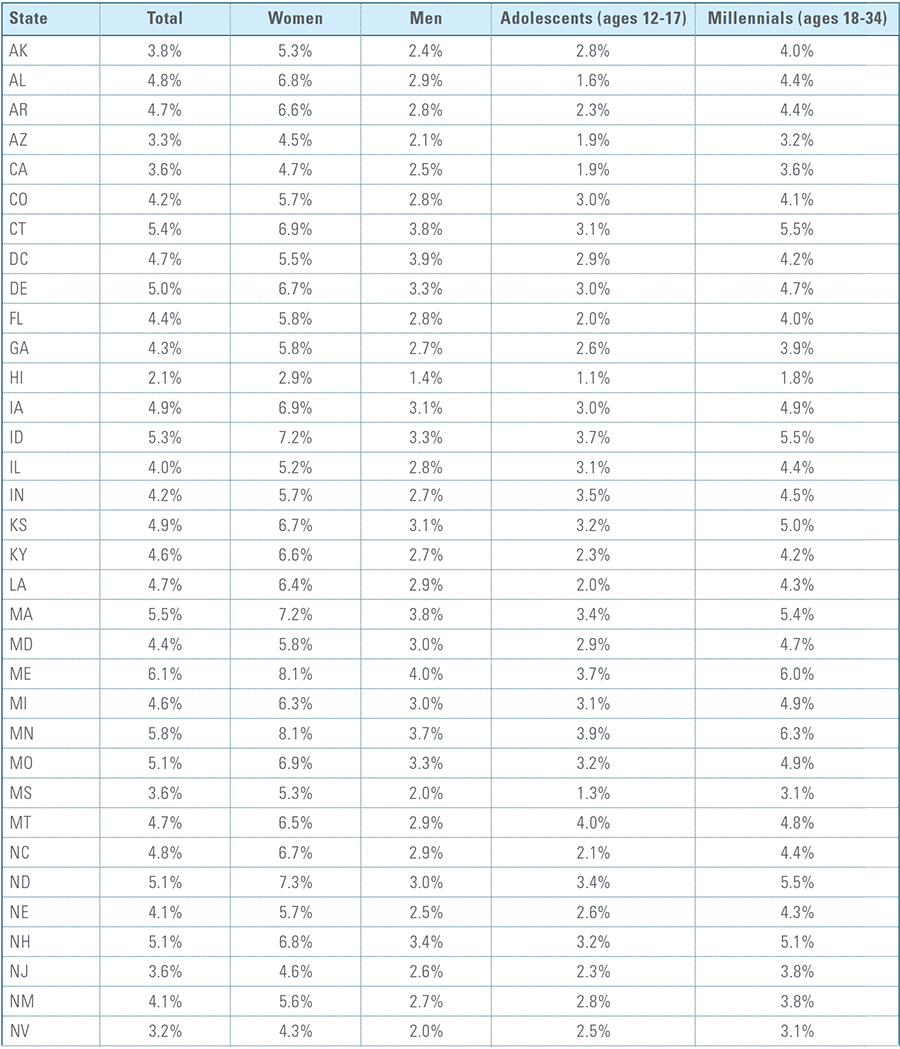
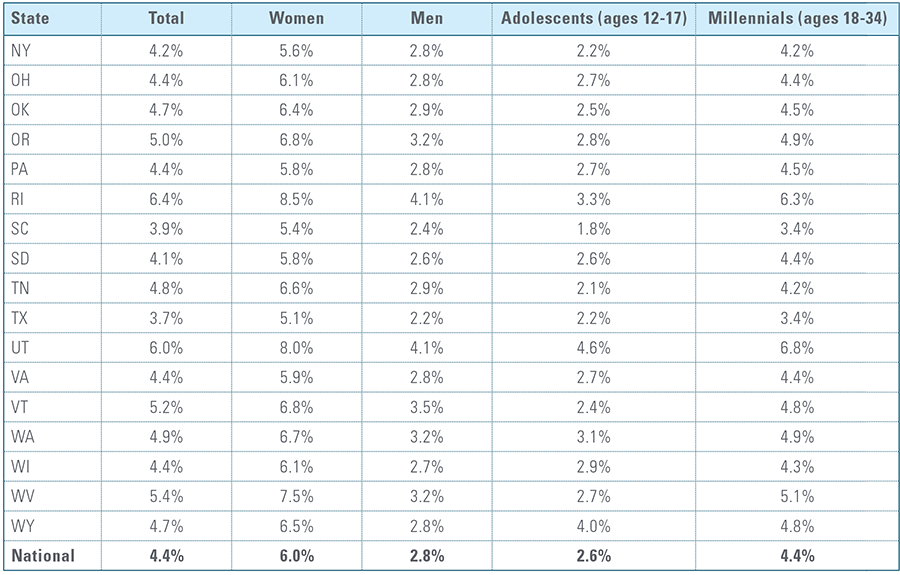
Appendix B:
Depression Diagnosis Rates by State (2016)
Appendix C:
Depression Diagnosis Rates by MSA (2016)*
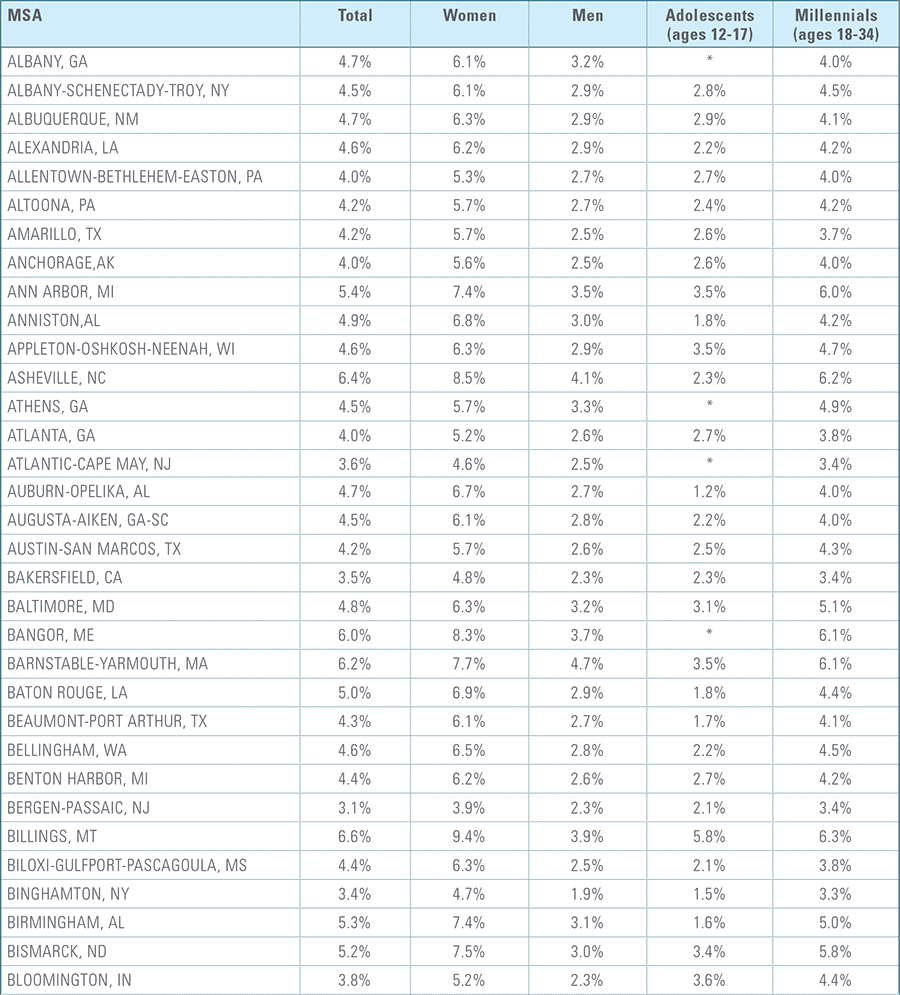
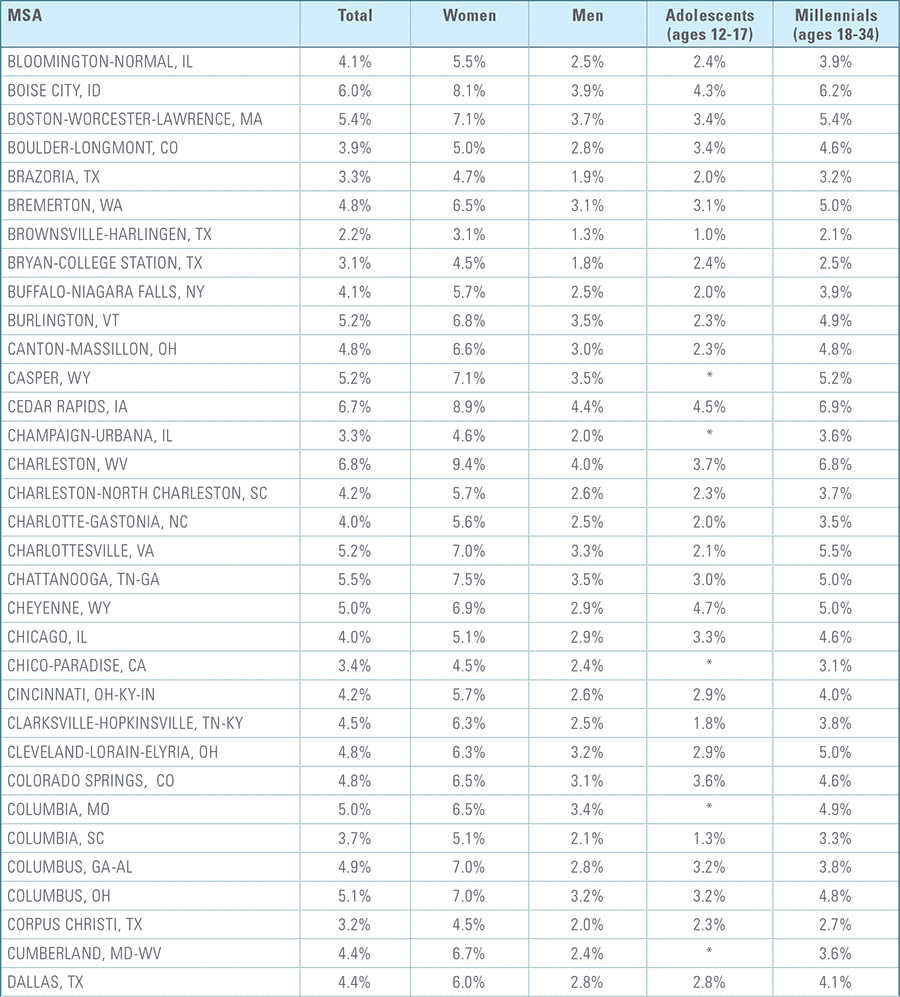
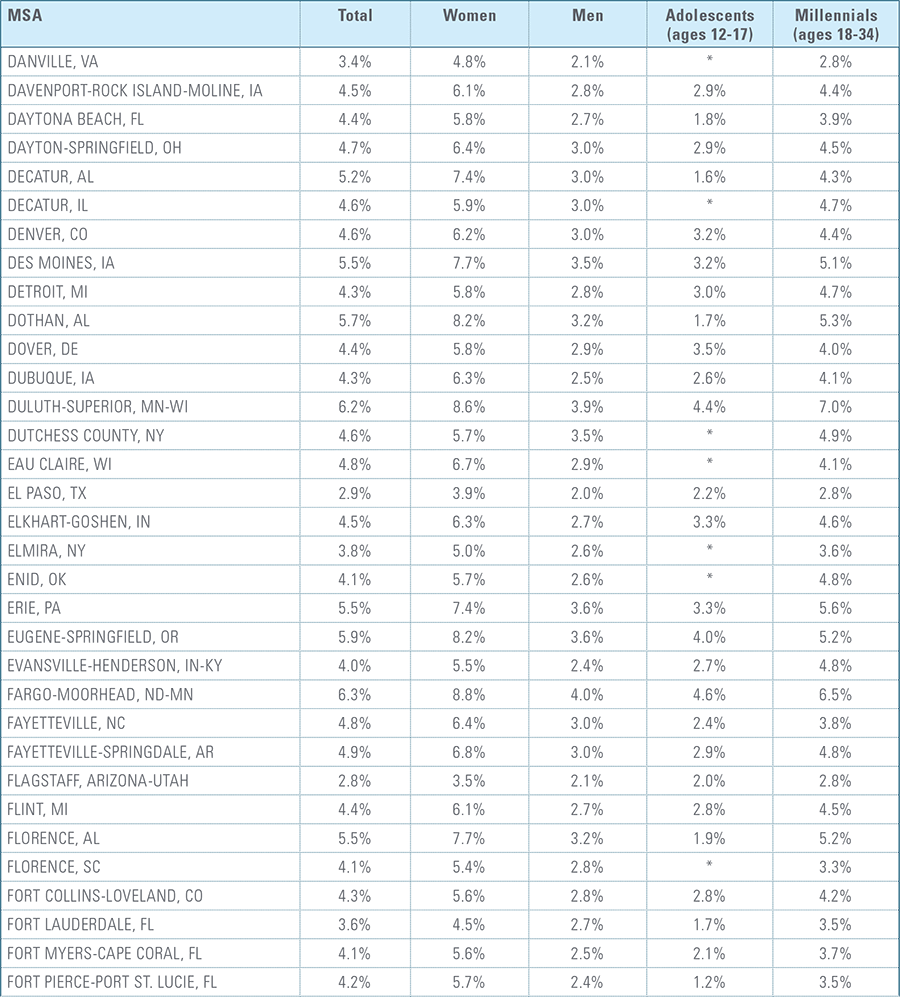
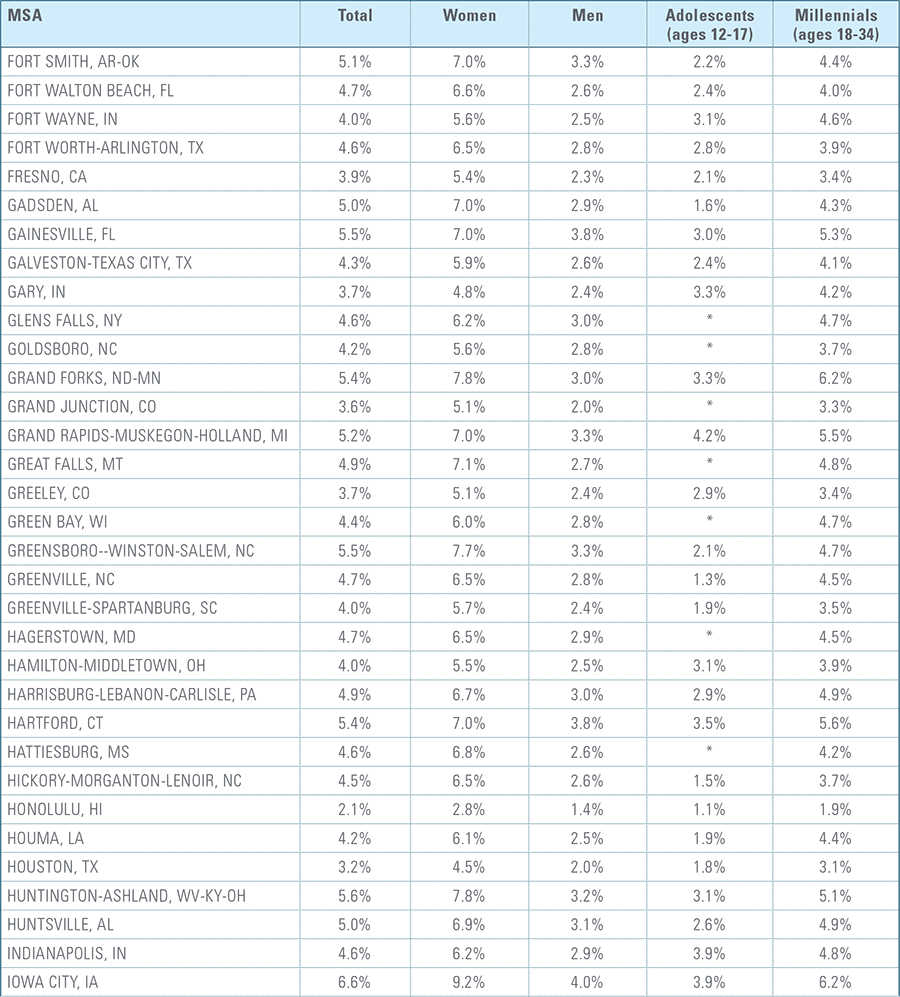
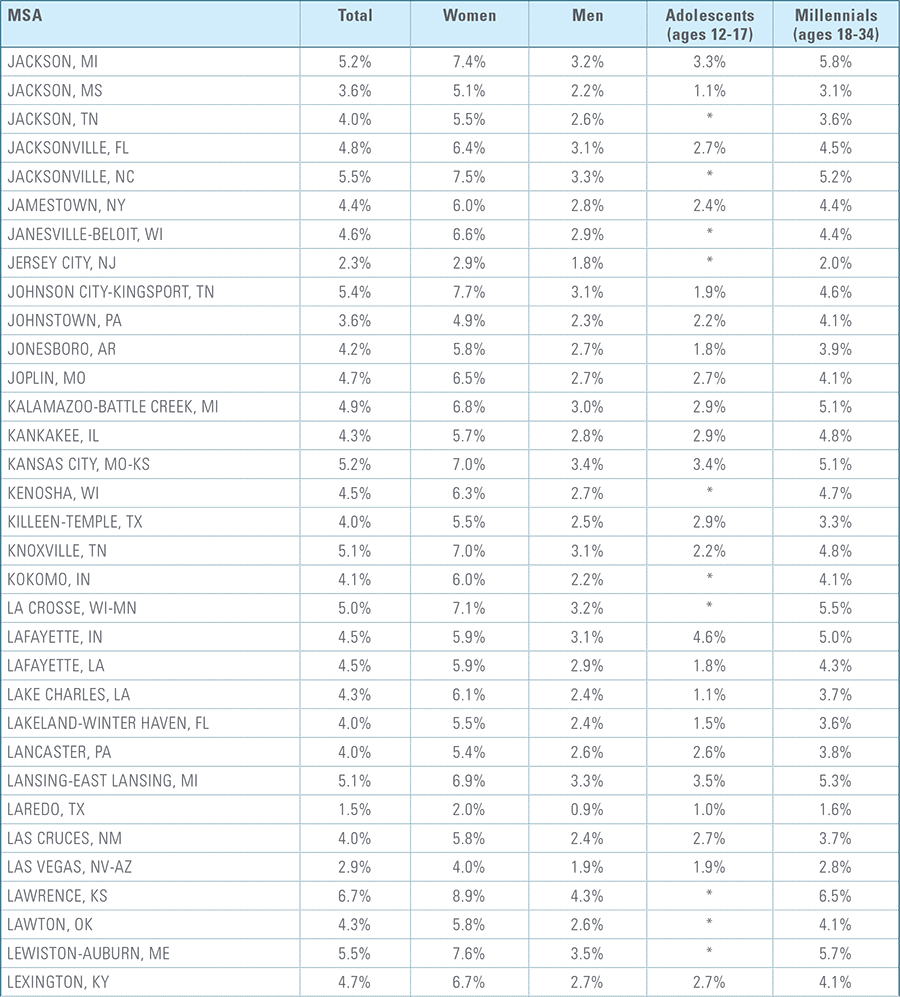
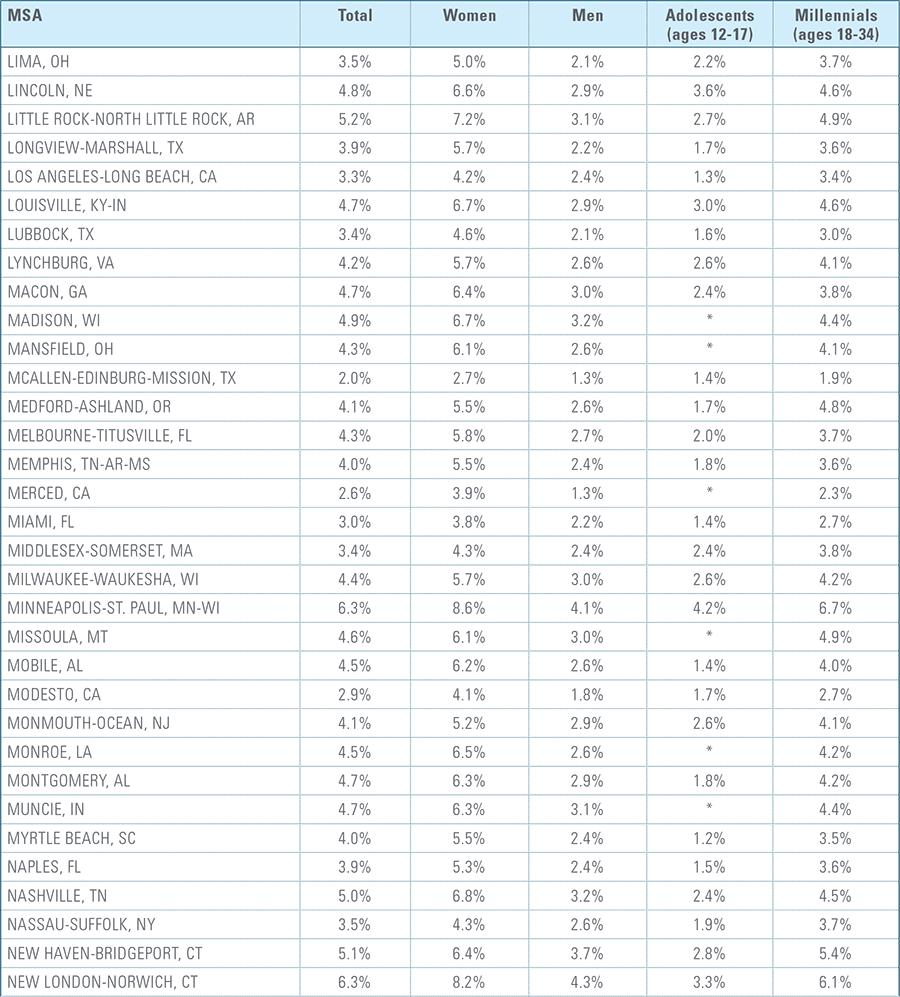
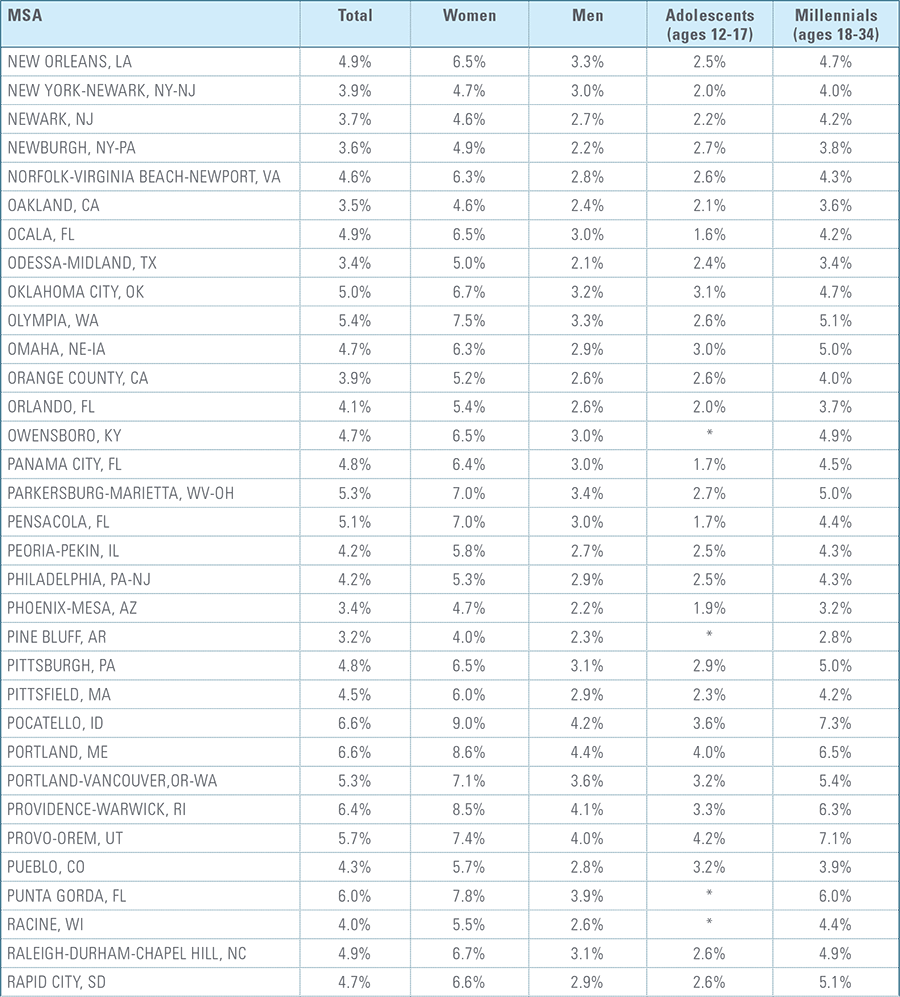
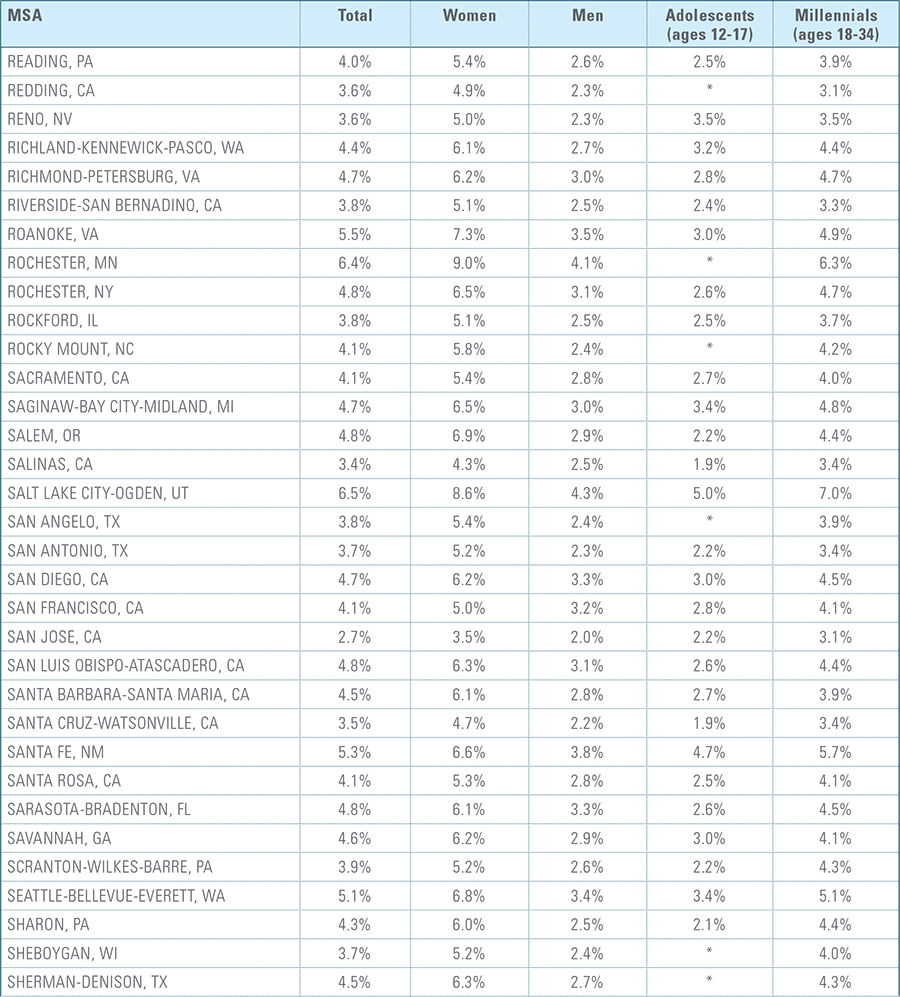
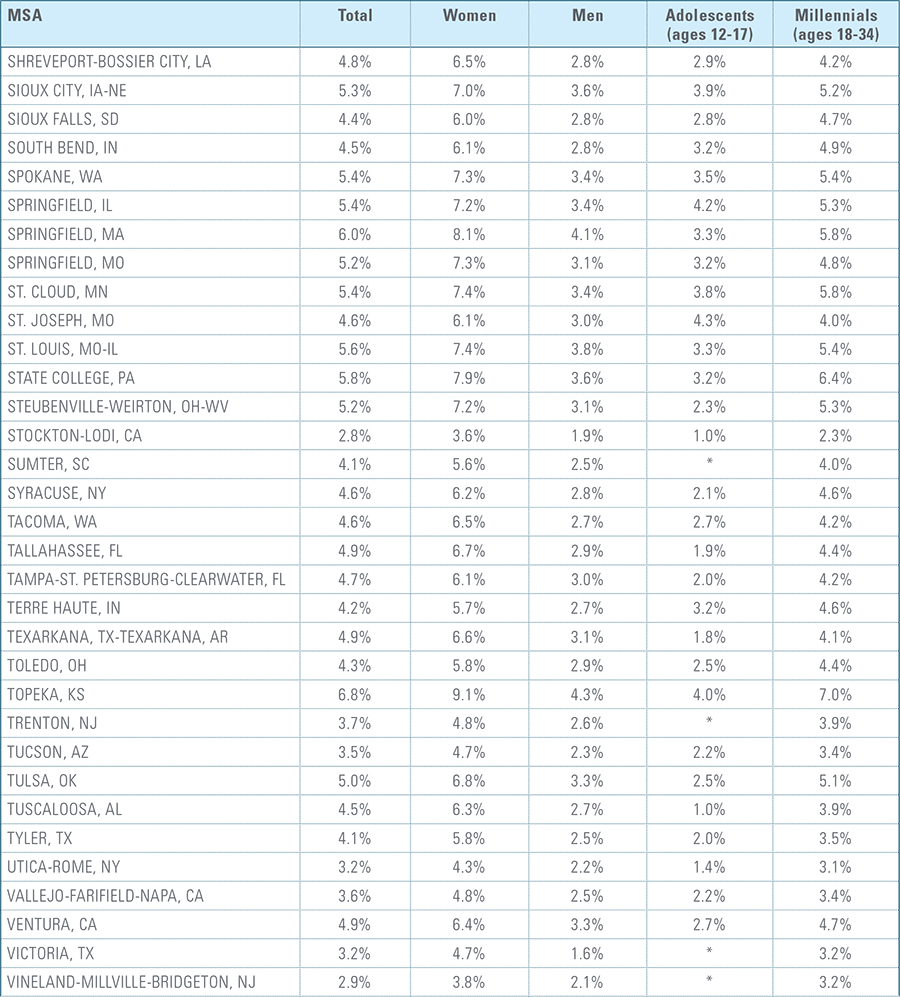
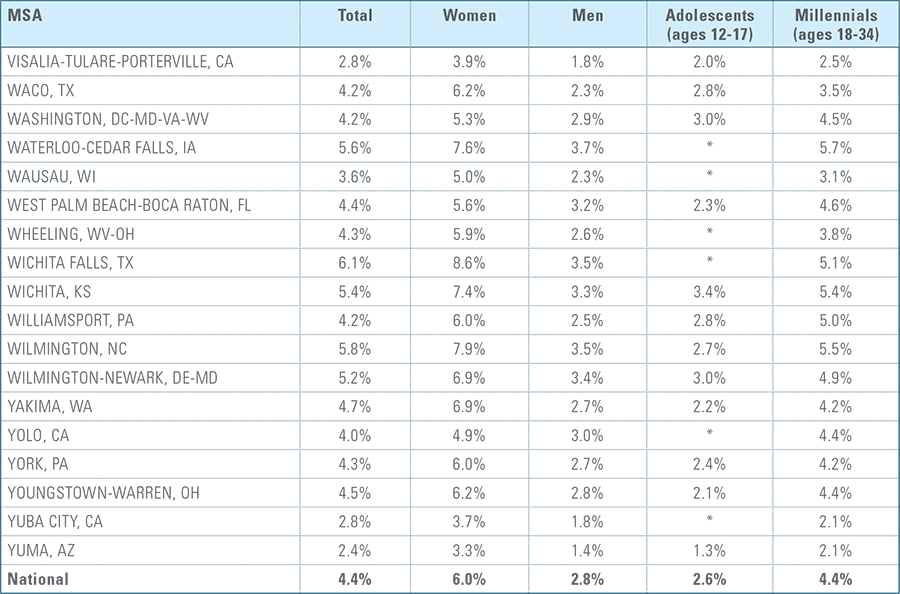
*MSAs must have data from at least 5,000 members to be included for total diagnosis rates and 1,500 members for demographic breakouts.

