| State and City |
Adjusted Cesarean Rate |
|---|
| Florida, Miami |
49.6% |
| Mississippi, Jackson |
49.6% |
Texas, McAllen-Edinburg-Mission,
Brownsville-Harlingen |
48.8% |
| South Carolina, Myrtle Beach/Florence |
46.2% |
| Florida, Fort Lauderdale |
45.0% |
| Michigan, Flint |
42.5% |
| New Jersey, Bergen-Passaic |
42.0% |
| Alabama, Mobile |
41.3% |
| Arkansas, Little Rock |
41.0% |
| New York, Nassau-Suffolk |
40.9% |
| Florida, West Palm Beach |
40.8% |
| Florida, Orlando |
40.4% |
| Tennessee, Memphis |
40.2% |
| Kentucky, Lexington |
40.2% |
| Alabama, Birmingham |
40.1% |
| Alabama, Montgomery |
40.1% |
| Alabama, Decatur-Florence |
39.8% |
| Texas, Dallas-Sherman-Denison |
39.7% |
| New Jersey, Newark |
39.5% |
| Alabama, Huntsville |
39.2% |
| Texas, Houston |
39.2% |
| Tennessee, Johnson City-Kingsport |
39.1% |
| South Carolina, Columbia |
39.0% |
| Georgia, Atlanta |
38.6% |
| Florida, Tampa-St. Petersburg |
38.5% |
| Kentucky, Louisville |
38.5% |
| Alabama, Tuscaloosa |
38.4% |
| Georgia, Columbus |
38.4% |
| Michigan, Saginaw-Bay City-Midland |
38.2% |
| Pennsylvania, Erie |
38.2% |
| Oklahoma, Tulsa |
38.1% |
| West Virginia, Huntington-Ashland |
37.9% |
| South Carolina, Greenville-Spartanburg |
37.9% |
| Tennessee, Nashville |
37.5% |
| New Jersey, Middlesex-Somerset |
37.4% |
| Virginia, Richmond-Petersburg |
37.4% |
| Florida, Jacksonville |
37.3% |
| North Carolina, Fayetteville |
37.3% |
| Connecticut, New Haven-Bridgeport |
37.1% |
| Oklahoma, Oklahoma City |
37.0% |
| North Carolina, Hickory-Morganton |
37.0% |
| Texas, Fort Worth-Arlington |
36.1% |
| South Carolina, Charleston |
36.1% |
| Texas, San Antonio |
36.1% |
| Tennessee, Chattanooga |
36.1% |
| New Jersey, Monmouth-Ocean |
36.1% |
| California, Modesto-Merced |
36.0% |
| District Of Columbia, Washington |
36.0% |
| California, Riverside-San Bernardino |
36.0% |
| Missouri, St. Louis |
35.8% |
| Ohio, Cincinnati |
35.8% |
| Michigan, Detroit-Ann Arbor |
35.8% |
| Pennsylvania, Scranton-Wilkes-Barre |
35.7% |
Tennessee,
Nashville/Clarksville-Hopkinsville |
35.6% |
| New York, New York |
35.6% |
| California, Los Angeles-Long Beach |
35.6% |
| Texas, Odessa-Midland |
35.4% |
| Tennessee, Knoxville |
35.3% |
| Virginia, Roanoke |
35.2% |
| Michigan, Lansing-East Lansing |
35.1% |
| Indiana, Indianapolis |
34.9% |
| Indiana, Gary |
34.8% |
| Ohio, Dayton-Springfield |
34.8% |
| Texas, Austin-San Marcos |
34.8% |
| Florida, Gainesville |
34.6% |
| Pennsylvania, Philadelphia |
34.5% |
| Florida, Pensacola/Fort Walton Beach |
34.5% |
North Carolina,
Rocky Mount/Greenville |
34.5% |
| Connecticut, Hartford |
34.4% |
| Pennsylvania, Sharon |
34.4% |
| Arkansas, Fayetteville-Springdale |
34.4% |
| Iowa, Sioux City |
34.2% |
| Maryland, Baltimore |
34.1% |
| California, San Diego |
34.0% |
| North Carolina, Charlotte-Gastonia |
33.9% |
| Virginia, Norfolk-Virginia Beach |
33.9% |
| Nebraska, Lincoln |
33.7% |
| Michigan, Grand Rapids-Muskegon |
33.6% |
| California, San Jose |
33.5% |
| North Carolina, Asheville |
33.4% |
| Pennsylvania, Lancaster |
33.4% |
| Pennsylvania, Allentown-Bethlehem |
33.3% |
North Carolina,
Greensboro-Winston-Salem |
33.2% |
| Michigan, Kalamazoo-Battle Creek |
33.1% |
| Rhode Island, Providence-Warwick |
33.0% |
| Delaware, Wilmington-Newark |
32.9% |
| California, Orange County |
32.8% |
| Nebraska, Omaha |
32.5% |
| Arizona, Phoenix-Mesa |
32.4% |
| Iowa, Des Moines |
32.2% |
| Pennsylvania, Pittsburgh |
32.2% |
| Illinois, Chicago |
32.1% |
| North Dakota, Bismarck |
31.8% |
| Washington, Portland-Vancouver |
31.8% |
| Ohio, Columbus |
31.6% |
Washington,
Seattle-Bellevue-Everett-Bellingham |
31.5% |
| Indiana, Fort Wayne |
31.5% |
| Pennsylvania, Harrisburg-Lebanon |
31.4% |
| Iowa, Cedar Rapids |
31.4% |
| Pennsylvania, York |
31.1% |
| New York, Albany-Schenectady-Troy |
31.0% |
| Kansas, Kansas City |
31.0% |
| Pennsylvania, Reading |
30.9% |
| Ohio, Cleveland-Lorain-Elyria |
30.9% |
North Carolina,
Raleigh-Durham-Goldsboro |
30.9% |
California,
Oakland/Vallejo-Fairfield-Napa |
30.5% |
| New York, Buffalo-Niagara Falls |
30.5% |
| Massachusetts, Boston-Worcester |
30.3% |
| Minnesota, Grand Forks |
30.2% |
| Iowa, Davenport-Moline |
29.6% |
| Washington, Tacoma-Bremerton |
29.5% |
| California, San Francisco |
28.6% |
| Colorado, Denver |
28.5% |
| Minnesota, Minneapolis-St. Paul |
28.4% |
| Wisconsin, Milwaukee-Waukesha |
28.2% |
| South Dakota, Sioux Falls |
28.0% |
| Idaho, Boise City |
27.6% |
| North Dakota, Fargo-Moorhead |
27.5% |
| Hawaii, Honolulu |
27.1% |
| Utah, Salt Lake City-Ogden |
27.1% |
| Iowa, Iowa City |
23.7% |
| New Mexico, Albuquerque |
22.7% |
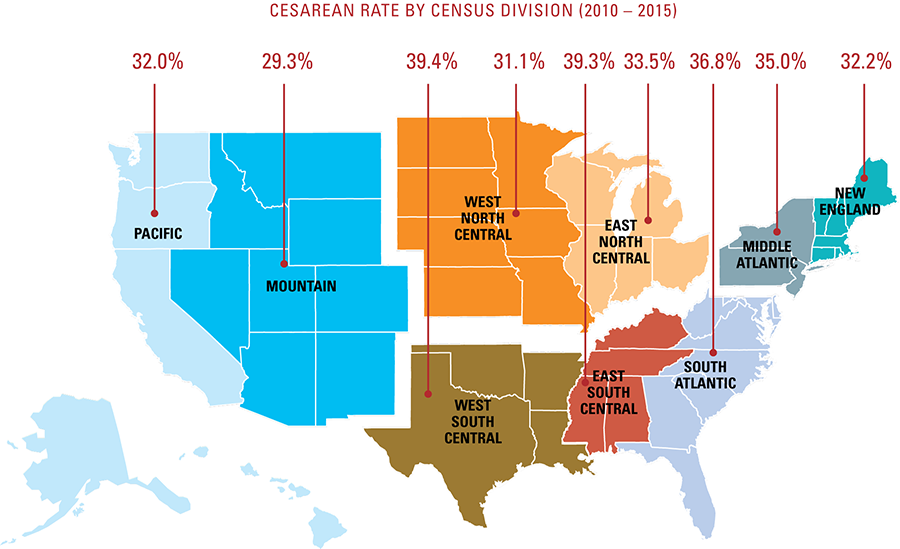
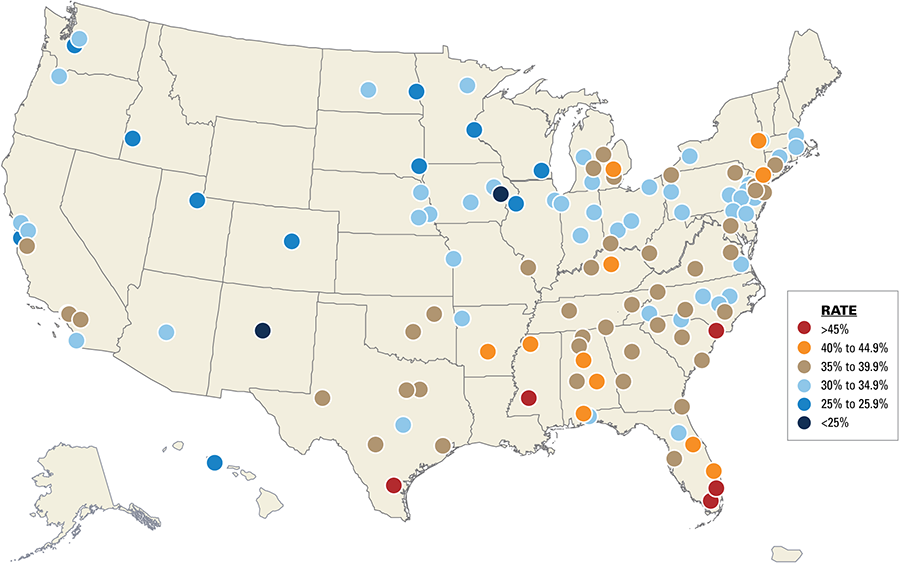
 The likelihood that an expectant mother will have a cesarean delivery1 is determined in large part by where she lives. An analysis of Blue Cross and Blue Shield (BCBS) companies’ data taken from 3 million deliveries by BCBS commercially-insured members shows that the rate of cesarean deliveries is more than twice as high in some parts of the country than in other parts and that even rates by U.S. Census Division vary by as much as 35 percent.
The likelihood that an expectant mother will have a cesarean delivery1 is determined in large part by where she lives. An analysis of Blue Cross and Blue Shield (BCBS) companies’ data taken from 3 million deliveries by BCBS commercially-insured members shows that the rate of cesarean deliveries is more than twice as high in some parts of the country than in other parts and that even rates by U.S. Census Division vary by as much as 35 percent.

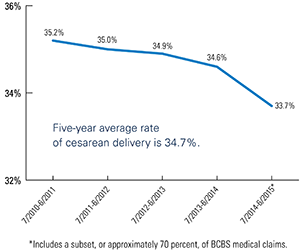 While geographic variation in cesarean deliveries is stark, the trend nationally may be shifting back toward vaginal deliveries. During a five-year period between July 2010 and June 2015, the cesarean rate decreased slightly each year within the BCBS population, to 33.7 percent from 35.2 percent. While small, this decline is consistent for all five years and reverses 20 years of increasing cesarean rates. A 1.5 percentage point decrease represents approximately 36,000 vaginal deliveries compared with cesarean sections in the same period.
While geographic variation in cesarean deliveries is stark, the trend nationally may be shifting back toward vaginal deliveries. During a five-year period between July 2010 and June 2015, the cesarean rate decreased slightly each year within the BCBS population, to 33.7 percent from 35.2 percent. While small, this decline is consistent for all five years and reverses 20 years of increasing cesarean rates. A 1.5 percentage point decrease represents approximately 36,000 vaginal deliveries compared with cesarean sections in the same period. Each delivery record contained the mother’s age, which allowed for analysis of results by age bands for mothers ages 18 through 49. Not surprisingly, the cesarean rate steadily increases with age, with mothers ages 18 through 24 recording the lowest cesarean rate (26.8%) and those 45 through 49 showing the highest rate (62.6%). Mothers under 20 represent a small fraction of total deliveries, and mothers ages 25-29 and 30-34 comprise the two largest age groups by total deliveries. Again, a prior cesarean delivery strongly associates with having future cesarean deliveries.
Each delivery record contained the mother’s age, which allowed for analysis of results by age bands for mothers ages 18 through 49. Not surprisingly, the cesarean rate steadily increases with age, with mothers ages 18 through 24 recording the lowest cesarean rate (26.8%) and those 45 through 49 showing the highest rate (62.6%). Mothers under 20 represent a small fraction of total deliveries, and mothers ages 25-29 and 30-34 comprise the two largest age groups by total deliveries. Again, a prior cesarean delivery strongly associates with having future cesarean deliveries.