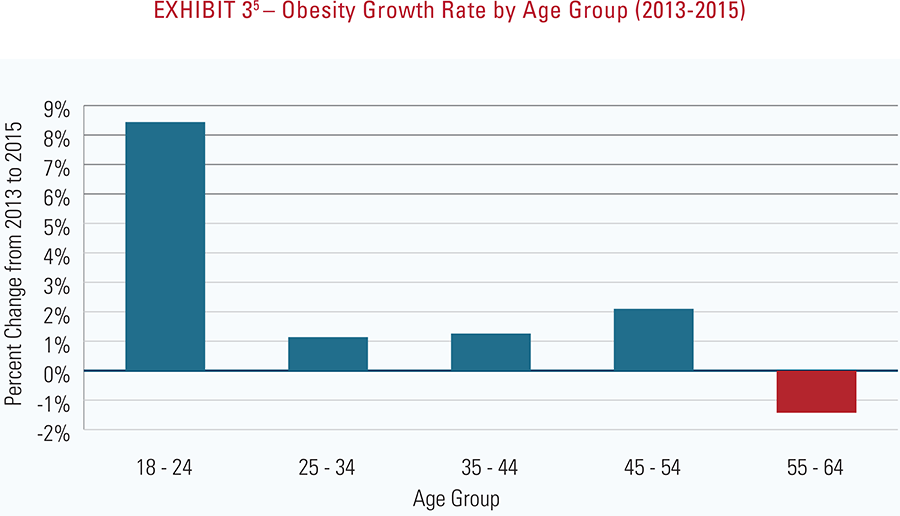I. Executive Summary
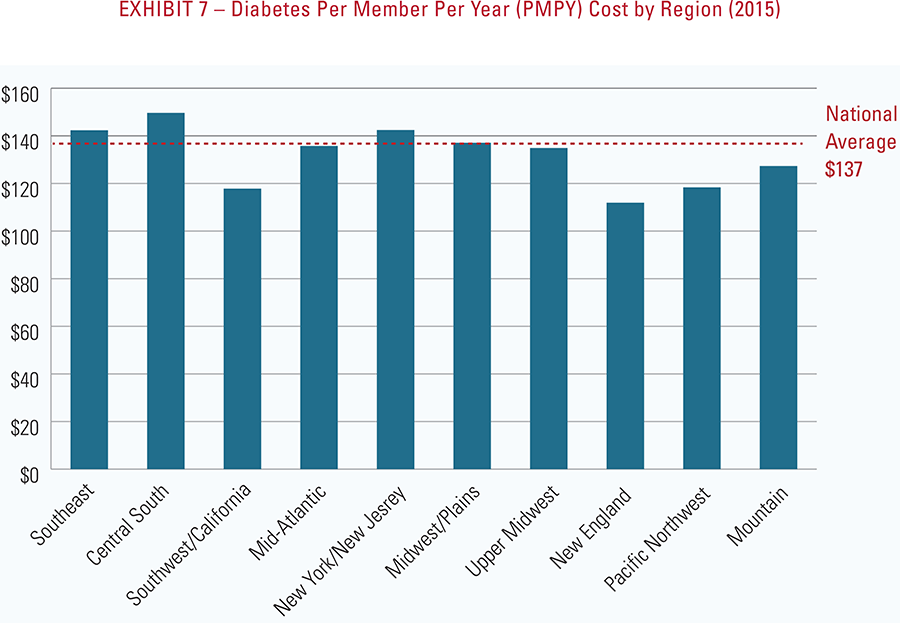
Diabetes is one of the diseases that most significantly impacts the health of America as reflected by nearly every national metric. Among the over 200 conditions measured by the BCBS Health Index, diabetes is third in terms of its health impact nationally on quality of life, and third in terms of per member cost for the commercially insured population. Its impact on health is even greater when considering common comorbid conditions such as hypertension (present in 93% of diabetics), high cholesterol (81%), obesity (55%) and others.1
Key Findings from the BCBS Health Index:
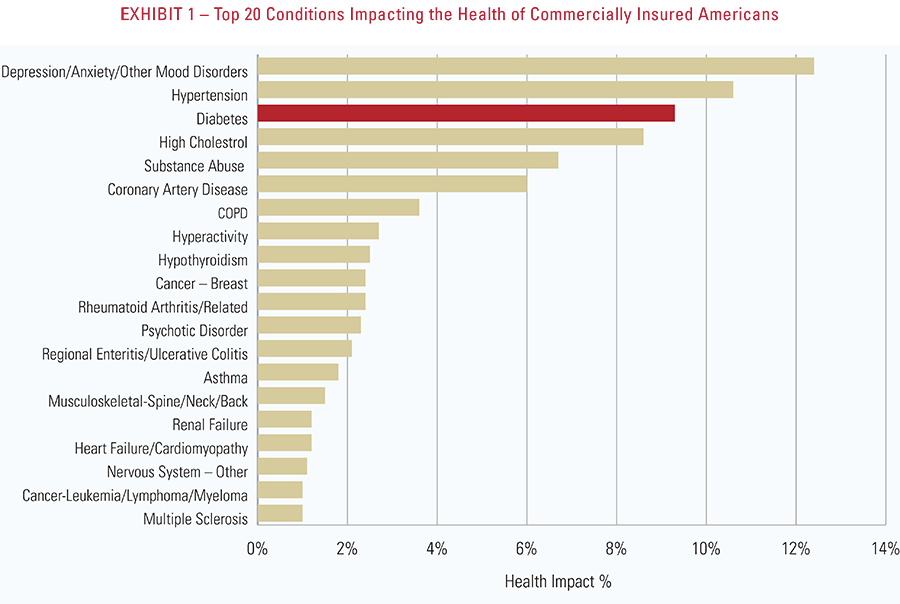
- Diabetes accounts for 9.3% of the health impact of over 200 conditions on commercially insured Americans—greater than heart disease, substance abuse and COPD.
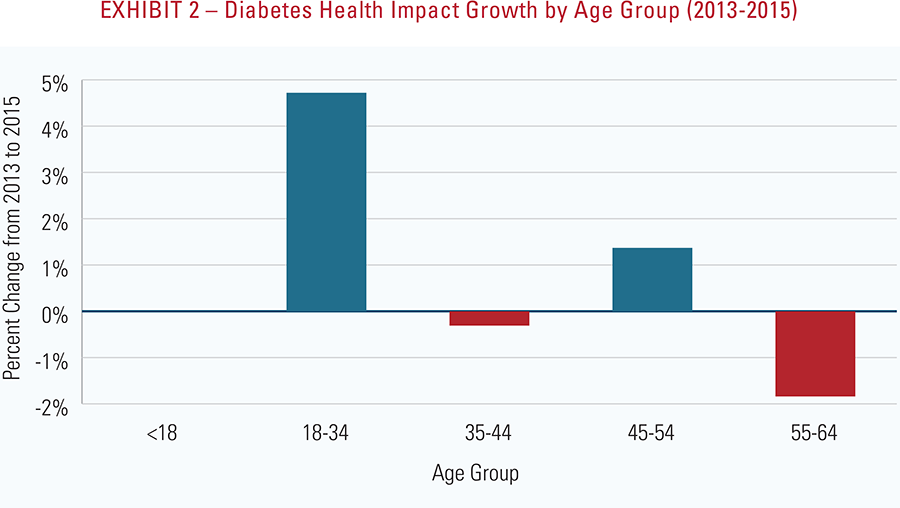
- The impact of diabetes continues to grow and it is increasing most rapidly in the 18-34 age group, corresponding to the fact that this young cohort is experiencing the greatest growth in obesity rates. Obesity is a key contributor to the onset of diabetes.
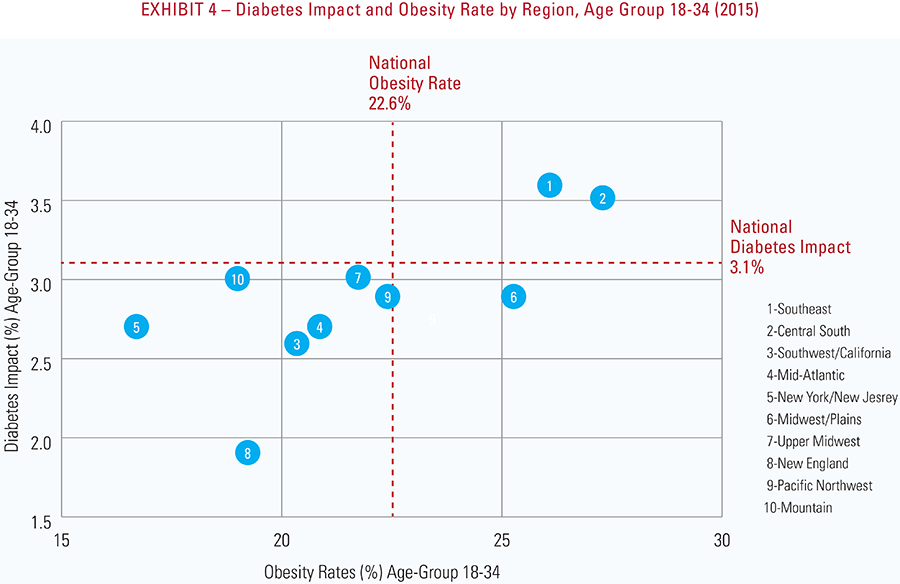
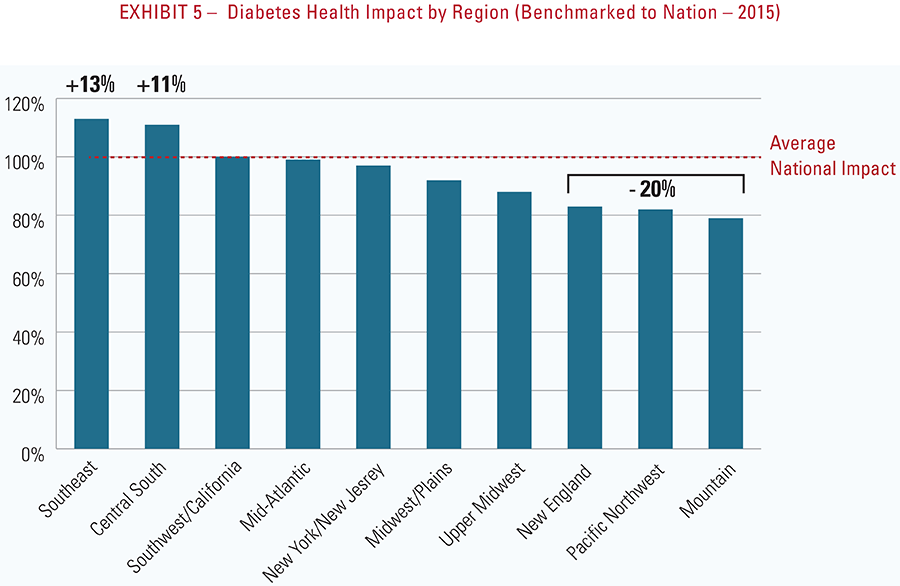
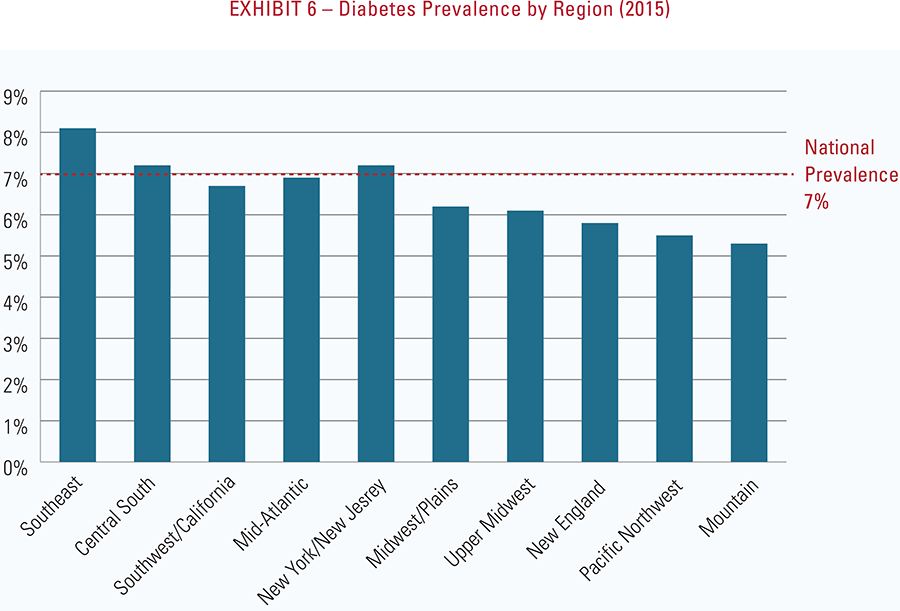
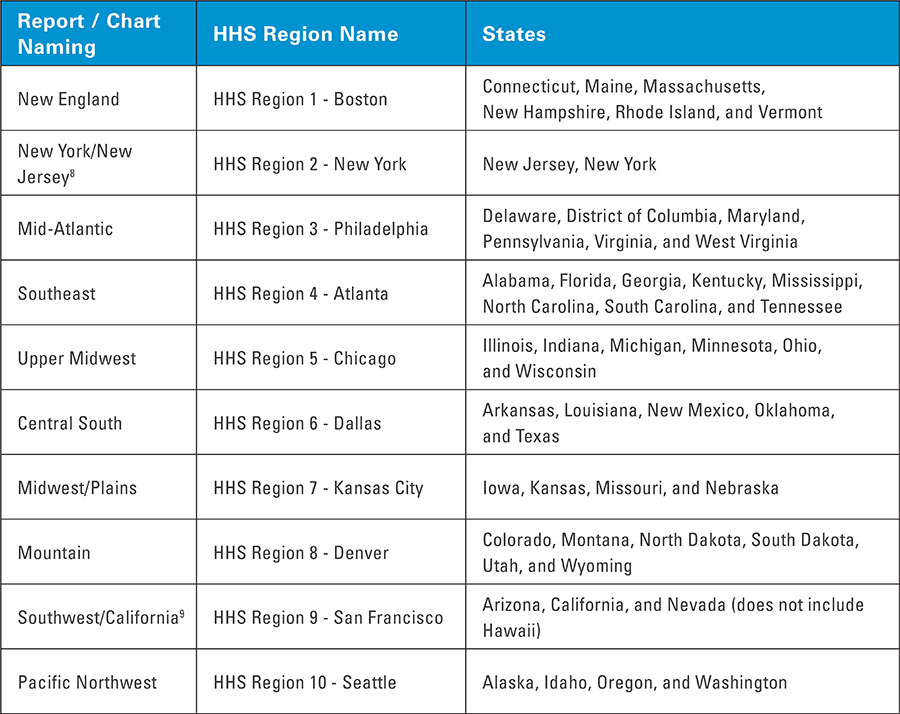
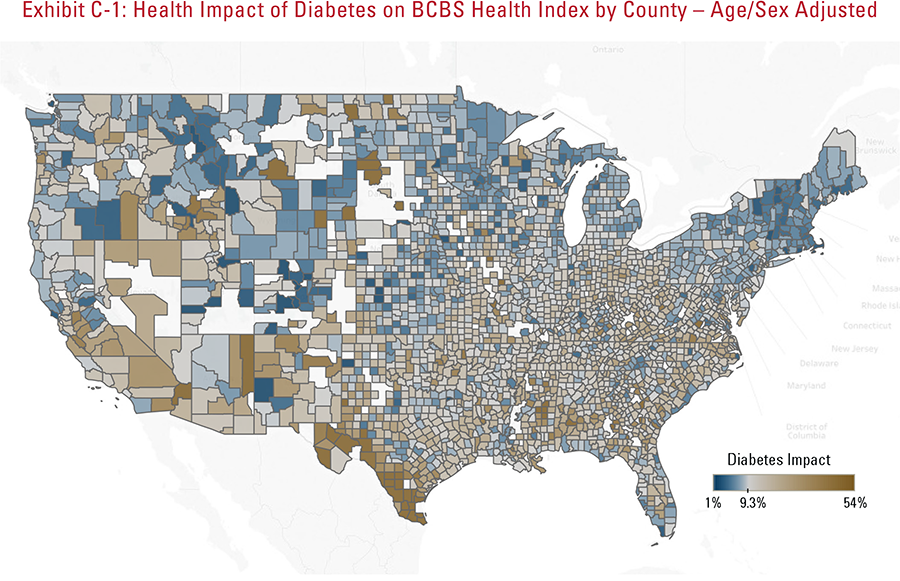
- Diabetes has the highest health impact on communities in the Southeast and Central South2—approximately 50% higher than the national average; the lowest diabetes impact is in New England and the Mountain regions.