Introduction
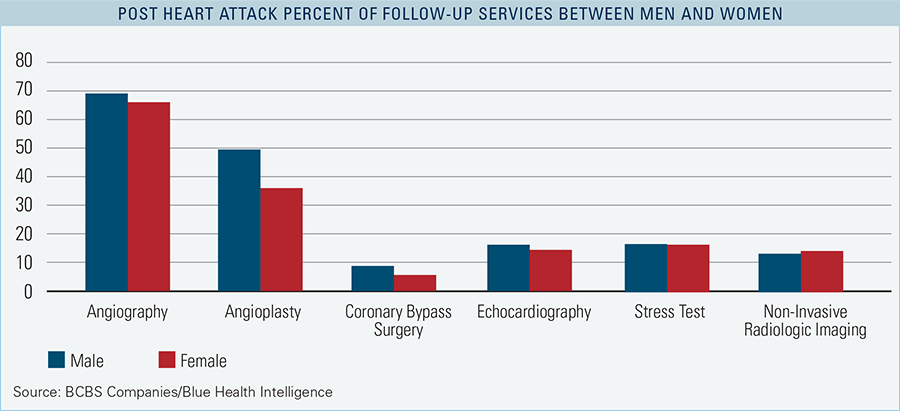
As healthcare moves towards personalized or precision medicine, the differences between women and men should play an increasingly important role in diagnosis and treatment. To explore the potential impact of these differences in healthcare, this report analyzed medical claims from Blue Cross and Blue Shield (BCBS) members to compare heart attack rates and treatment patterns between women and men in the United States. The results show that women are receiving less aggressive treatments after a heart attack than men. This pattern emerges even as a greater percentage of women than men die or become disabled due to heart attacks.1
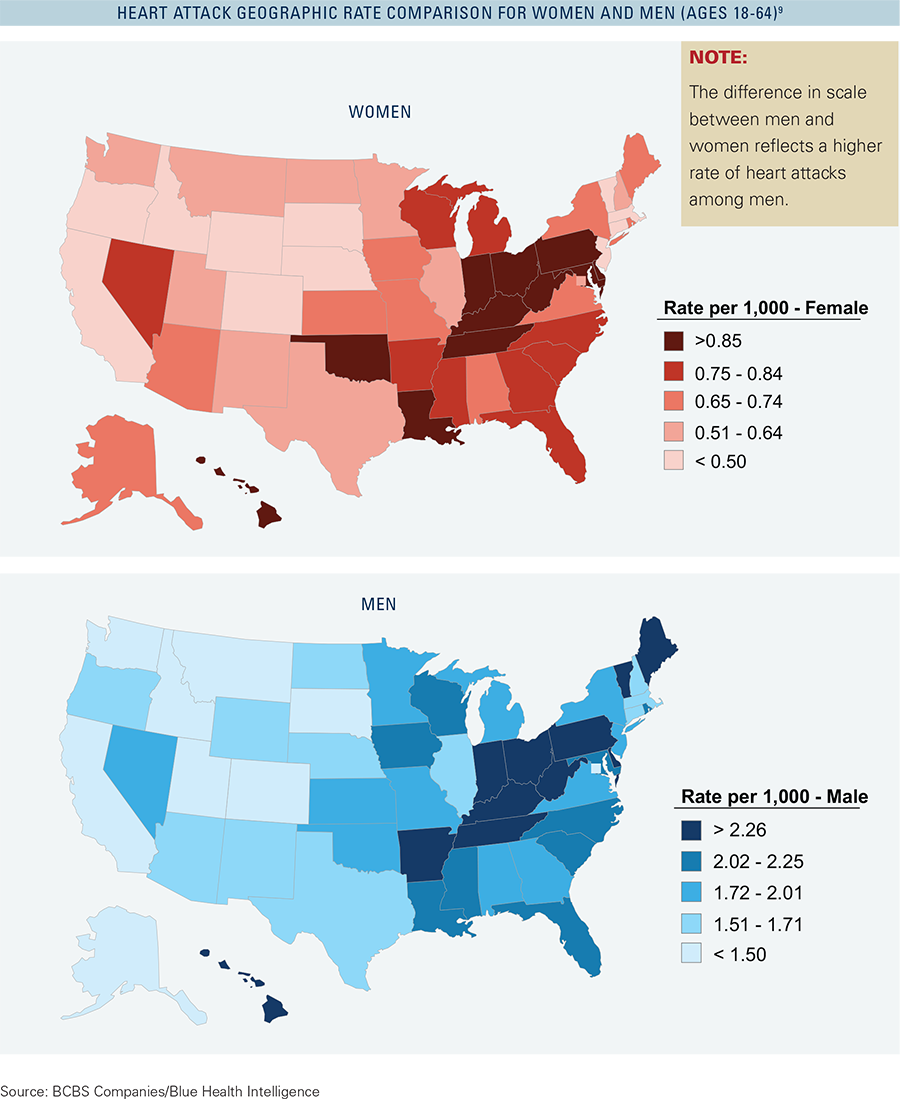
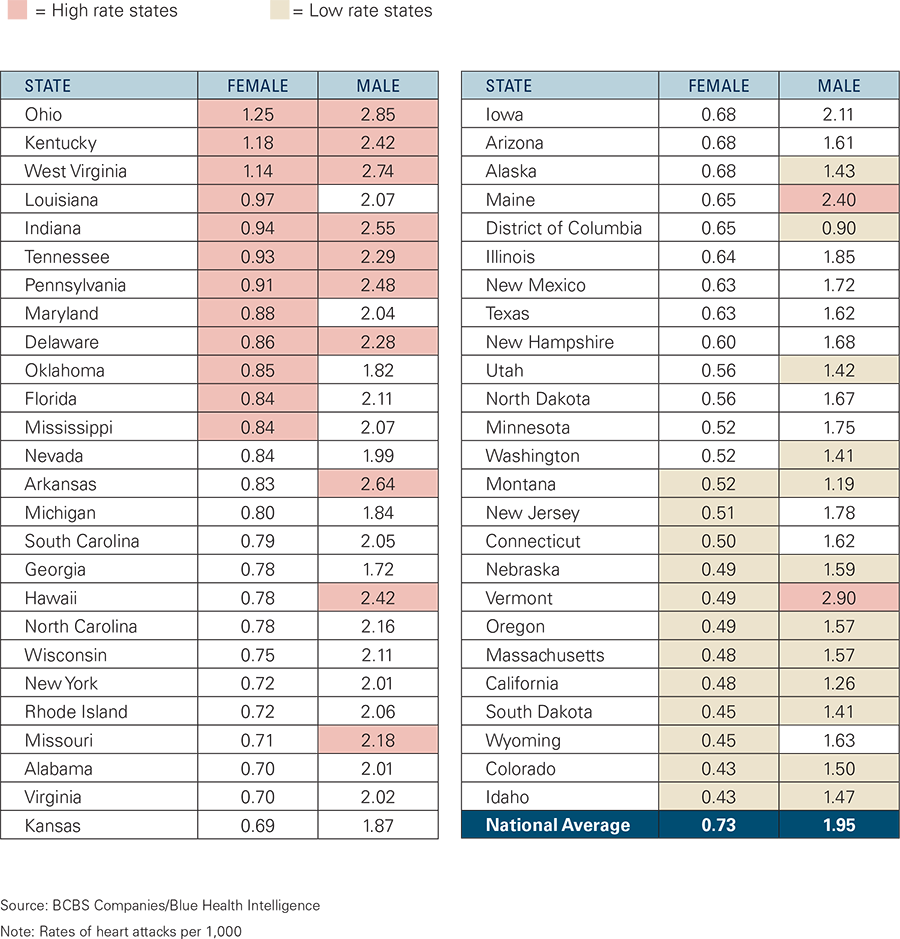
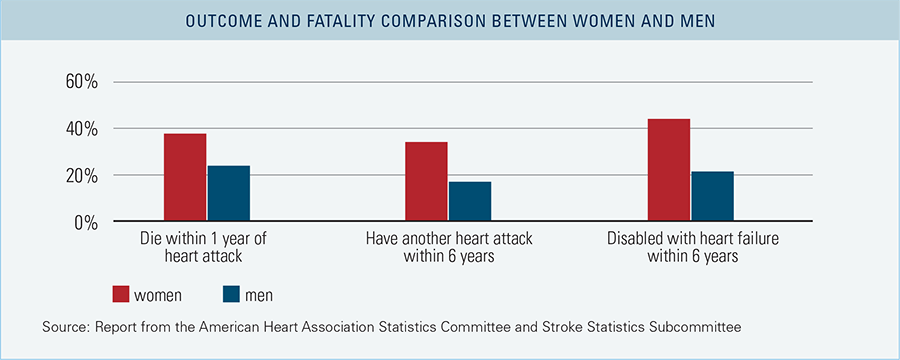
BCBS data reveals that heart attacks occur more frequently in men than women, a finding that is consistent with statistics reported by the Centers for Disease Control and Prevention. However, the American Heart Association reports that while heart disease and heart attacks are more prevalent in men, women who experience heart attacks have worse outcomes — they are more likely than men to die within one year of a heart attack, to have another heart attack within six years, and to be disabled because of heart failure within six years. In fact, heart disease far surpasses breast cancer and other recognized causes of death among U.S. women.2
Heart attacks place a significant physical and economic toll on Americans. They are the deadliest type of heart condition, accounting for nearly 40 percent of coronary heart disease-related deaths each year. Nearly 1.2 million heart attacks occur annually, 700,000 of which are for the first time. The calculated economic burden of heart disease is $133 billion in the United States.3 Heart attacks rank among the five most expensive conditions seen during inpatient hospitalizations in the U.S., accounting for total costs of over $11.5 billion and 612,000 hospital stays.4
This report intends to raise awareness of women’s heart health by analyzing BCBS data to show the following:

This analysis is based on 2014 claims data from independent BCBS companies’, focusing on people ages 18 through 64.5 The data set contains more than 43 million BCBS commercially insured members (excludes Medicare and Medicaid).
This is the third edition of “Blue Cross Blue Shield, The Health of America Report,” a collaboration between the Blue Cross Blue Shield Association and Blue Health Intelligence, which uses a market-leading claims database to uncover key trends and insights into healthcare affordability and access to care.