Trends in Pregnancy and Childbirth Complications in the U.S.

Millions of women give birth in the U.S. every year. A majority of these women have healthy pregnancies and deliveries. However, an analysis of Blue Cross Blue Shield data reveals an increasing number of women are experiencing pregnancy complications and childbirth complications.
This report examines 1.8 million pregnancies between 2014 and 2018 among commercially insured women ages 18-44.1 While the overall pregnancy rate has declined by 2% in this population since 2014, it varies considerably by age. The rate for women ages 18-24 declined by 12% while the rate for women ages 35-44 increased by 9%. While the average age of pregnancy increased over the study period from 30.6 to 31, childbirth complications did not increase with age.
Using our market-leading claims database, this report digs deeper into this population of women to gain a better understanding of their health before, during and after pregnancy. It also showcases how Blue Cross and Blue Shield companies are taking actions to improve women’s health across the country.
Related Content: Learn about how race and ethnicity influence pregnancy and childbirth risks in a September 2022 BCBS study that reveals disparities in Severe Maternal Morbidity (SMM).

The Health of Millennials report found double digit increases in millennials for 8 of the 10 top health conditions like major depression, hypertension and type II diabetes. Additionally, prevalence rates for these conditions are higher in millennials than in their Gen X counterparts at the same age.
Chronic Conditions are more Prevalent before Pregnancy
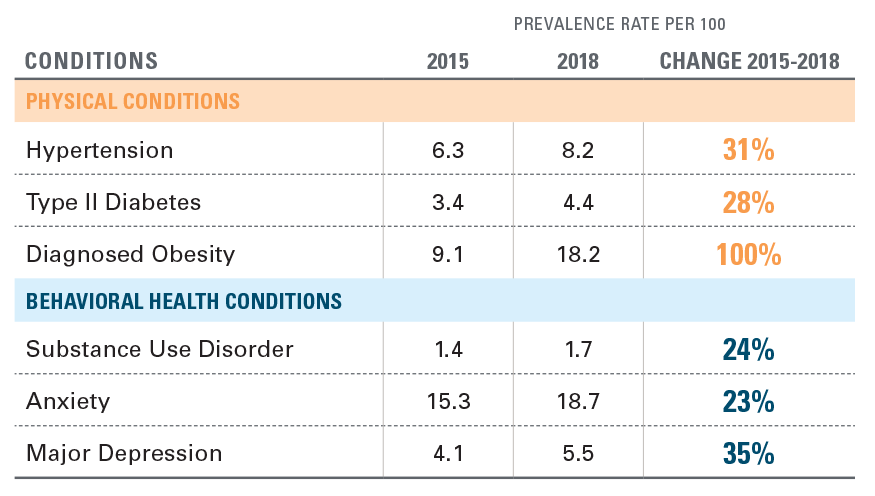
There was a significant increase in the prevalence of chronic physical and behavioral health conditions before becoming pregnant from 2015 to 2018,3 with the largest increases seen in diagnosed obesity and major depression (see Exhibit 1). Pre-existing conditions increase the risk of pregnancy complications and childbirth complications.
EXHIBIT 1: PREVALENCE OF PRE-EXISTING CONDITIONS PRIOR TO PREGNANCY, 2015-2018
Listen
Blue Cross & Blue Shield of Mississippi has embedded health coaches and nutritionists in OBGYN offices to help women manage chronic diseases and lead healthier lives.
LISTEN TO PODCAST
THE IMPACT OF COVID-192
Accessing prenatal care has changed for a majority of women since the start of the COVID-19 pandemic. 61% of the women surveyed saw limited office hours from their doctors and 48% had their prenatal appointments shifted to virtual visits.
More concerning is that over 1 in 4 women surveyed skipped prenatal appointments since the start of the pandemic or when social distancing restrictions were put into place.

Read
BlueCross BlueShield of Tennessee helped launch a major telemedicine network to serve rural women with high risk pregnancies.
READ MORE
Gestational Diabetes and Preeclampsia Driving Increase in Pregnant Complication Rates
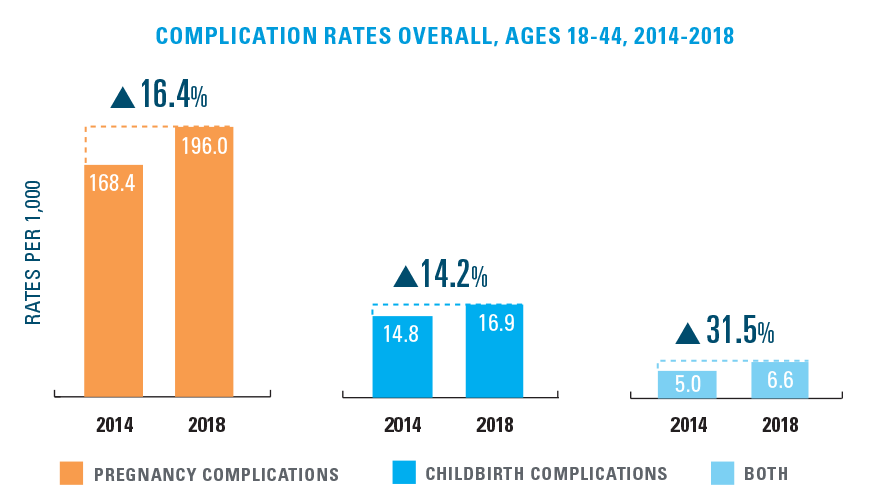
While 80% of women have healthy pregnancies and deliveries, rates of complications are rising. Between 2014-2018, the rates of pregnancy complications rose more than 16%, while rates for childbirth complications rose more than 14%. About seven out of every 1,000 pregnant women experienced both kinds of complications, a nearly 31% increase since 2014. Pregnancy complication rates were much higher for older women5 (see Exhibit 2).
EXHIBIT 2: OVERALL RATES OF PREGNANCY COMPLICATIONS AND CHILDBIRTH COMPLICATIONS BY AGE, 2014-2018

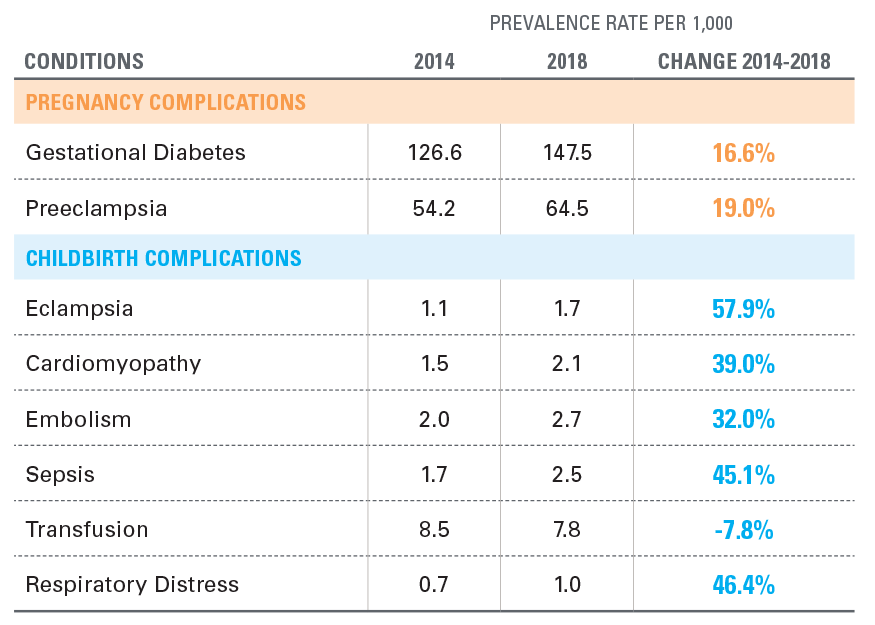
Among pregnancy complications, rates of both gestational diabetes and preeclampsia increased by double digits. For childbirth, rates of almost all complications but transfusion increased by double digits, as well. While rates of childbirth complications were low, the rates of these complications are increasing rapidly (see Exhibit 3).
EXHIBIT 3: PREGNANCY AND CHILDBIRTH COMPLICATIONS AMONG WOMEN 18- 44, 2014-2018

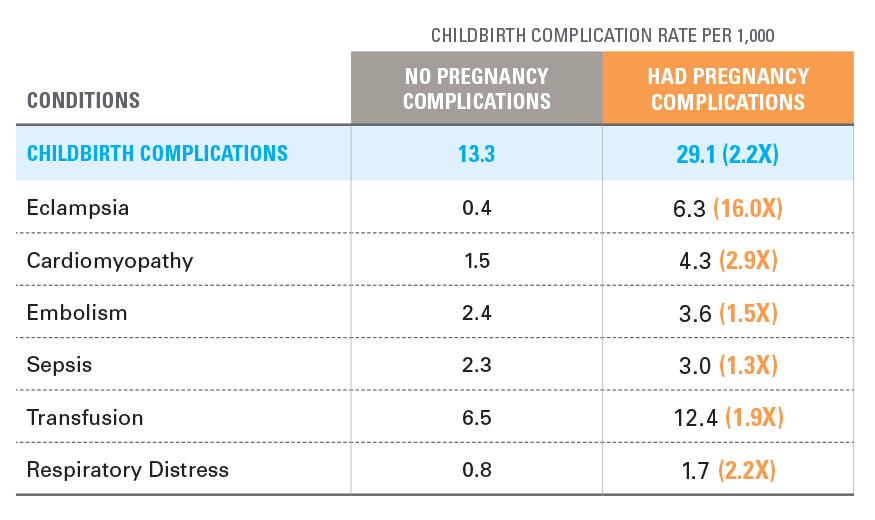
In addition, women who have complications during pregnancy, like gestational diabetes or preeclampsia, are twice as likely to have childbirth complications than women who did not have pregnancy complications.
EXHIBIT 4: RATES OF CHILDBIRTH COMPLICATIONS AMONG WOMEN WITH/WITHOUT PREGNANCY COMPLICATIONS IN 2018
Read
Working with OBGYNS, Blue Cross and Blue Shield of Alabama helps make regular prenatal care safe during COVID-19.
READ MORE
Rates of pregnancy complications and childbirth complications vary by state. These variations can be driven by a variety of factors like the overall health of women in those regions, provider practices, access to care and/or other social determinants of health.
THE IMPACT OF COVID-192
The COVID-19 pandemic impacted delivery plans for the majority of women surveyed:

Increases in Postpartum Depression
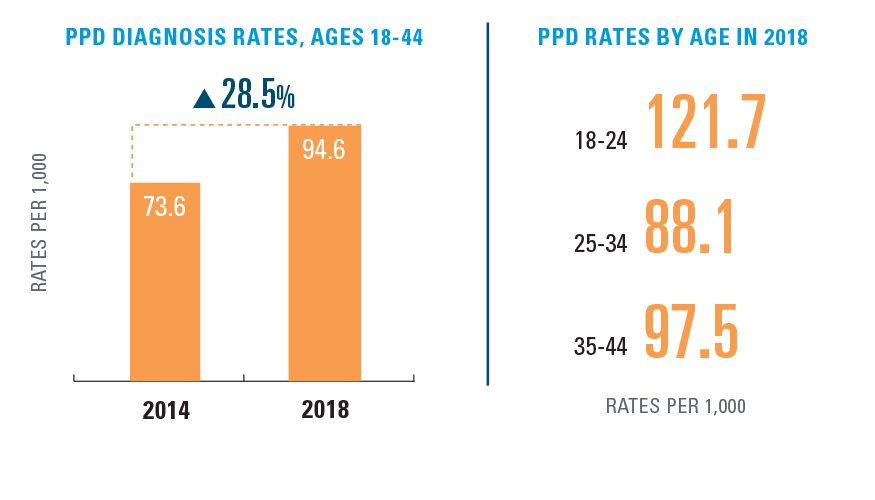
In 2018, nearly one in 10 women who delivered a baby was diagnosed with postpartum depression (PPD). That number is up almost 30% from 2014. Postpartum depression diagnoses were most prevalent in women aged 18-24. Some of this increase could be attributed to a greater awareness of the condition and more screening (see Exhibit 5).
EXHIBIT 5: RATE OF POSTPARTUM DEPRESSION (PPD) BY AGE, 2014-20187
Read
BlueCross & BlueShield of Rhode Island is providing resources for pediatricians to screen new mothers for postpartum depression and hire staff to connect them with treatment right away.
READ MORE

AT RISK FOR POSTPARTUM DEPRESSION
Pre-existing behavioral health conditions are linked with a greater risk for postpartum depression. More than two thirds of women diagnosed with postpartum depression had at least one other behavioral health diagnosis before becoming pregnant, and more than 1 in 4 women had two or more pre-existing behavioral health conditions.
TOP PRE-EXISTING BEHAVIORAL HEALTH CONDITIONS AMONG WOMEN DIAGNOSED WITH POSTPARTUM DEPRESSION:

THE IMPACT OF COVID-192
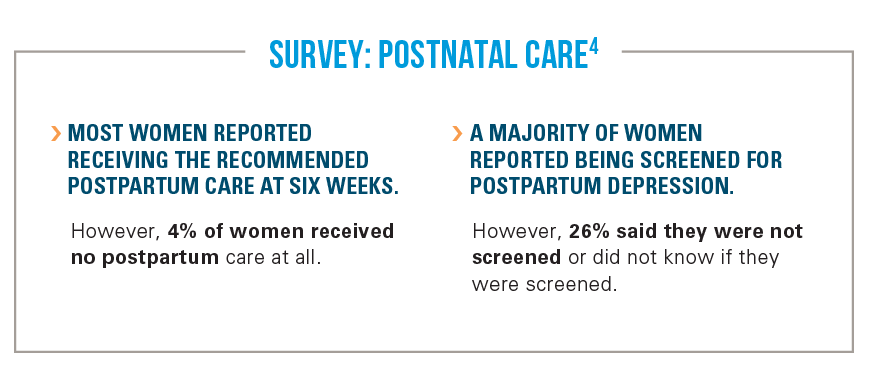
Postnatal care plans changed for a majority of women due to COVID-19. Over half said their doctor’s office hours are limited and
half have shifted to virtual visits. Additionally, a fifth of women missed their postnatal visits.

The Financial Impact of Pregnancy Complications and Childbirth Complications
In addition to having adverse health consequences, pregnancy complications and childbirth complications drive increased healthcare costs. Pregnancy complications increase the average cost of a vaginal delivery by 16% and a c-section delivery by 18%, while childbirth complications increase the average cost of these deliveries by 63% and 52% respectively.8
The Quality of Maternal Healthcare can Mitigate Risk and Cost
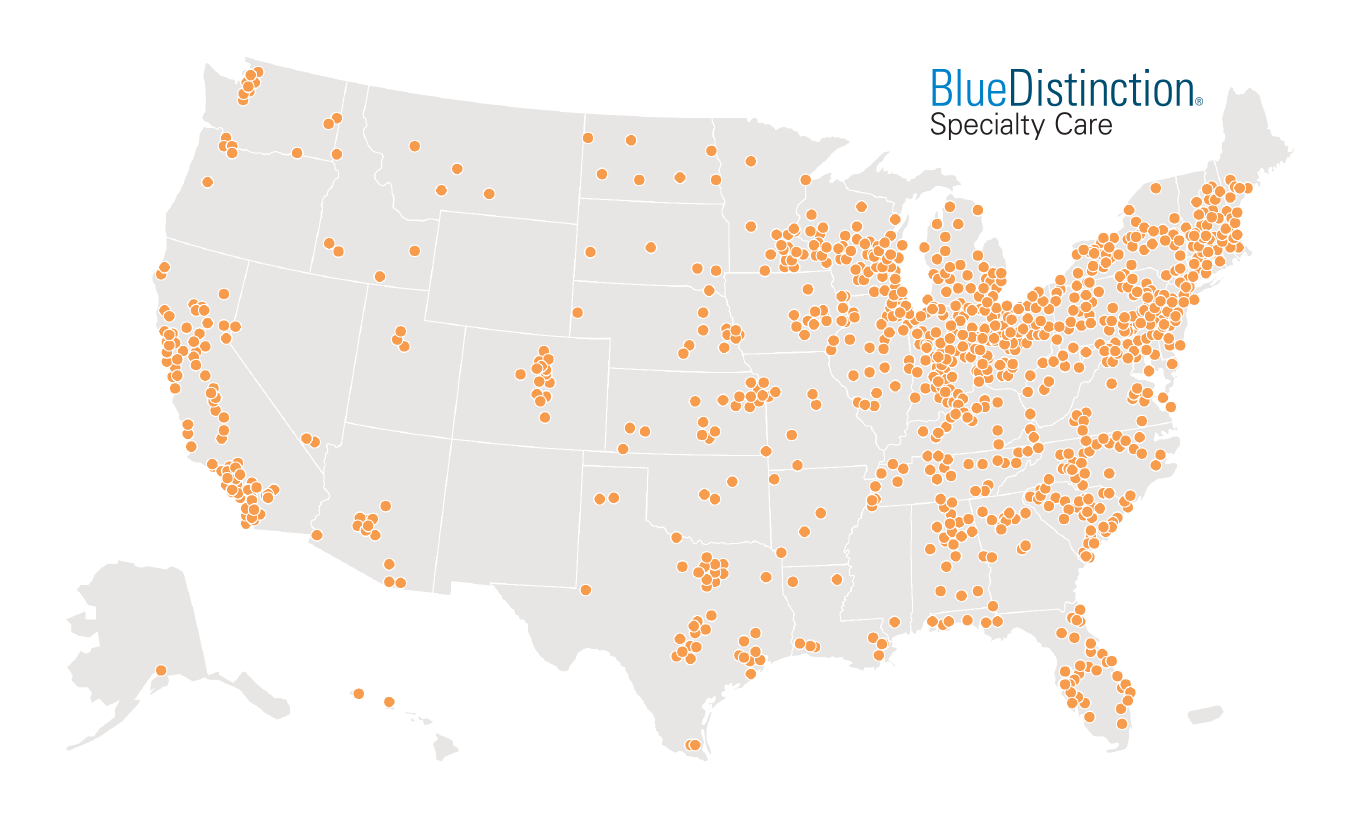
Blue Distinction Centers (BDC) and Blue Distinction Centers+ (BDC+) for Maternity Care are healthcare facilities and providers recognized for their demonstrated expertise delivering high quality, cost-effective care. In 2018, BDC/BDC+ facilities across the country cared for more than 40% of Blue Cross and Blue Shield commercially insured women giving birth. On average, BDC/BDC+ facilities cared for higher risk women while still maintaining comparable delivery outcomes to the national average and BDC+ facilities had significantly lower costs.9,10
EXHIBIT 6: >1,000 BLUE DISTINCTION CENTERS AND BLUE DISTINCTION CENTERS+ FOR MATERNITY CARE11
Conclusion
This report underscores the importance of focusing on the health of pregnant women in America, especially as health conditions increase in this population—increasing the likelihood of complications during pregnancy and childbirth as well as diagnoses of postpartum depression. Access to quality care is critical to helping women lead healthier lives, have healthier pregnancies and uncomplicated births. Blue Cross and Blue Shield companies across the country are making maternal health a priority in their communities—for the Health of America.SM
Methodology
This is the 31st study of the Blue Cross Blue Shield, The Health of America Report® series, a collaboration between Blue Cross Blue Shield Association and Blue Health Intelligence (BHI), which uses a market-leading claims database to uncover key trends and insights in healthcare affordability and access to care. This report analyzes the data of over 1.8 million pregnancy episodes between 2014 and 2018. Pregnancy episodes were identified by TEG grouper, including both those ending with a delivery and those without a delivery.
This report studies pregnancy and childbirth complications as well as chronic conditions affecting the health of pregnant women, using an integrated dataset combining the pregnancy episodes data curated from BCBS Axis Data and the BCBS Health Index.
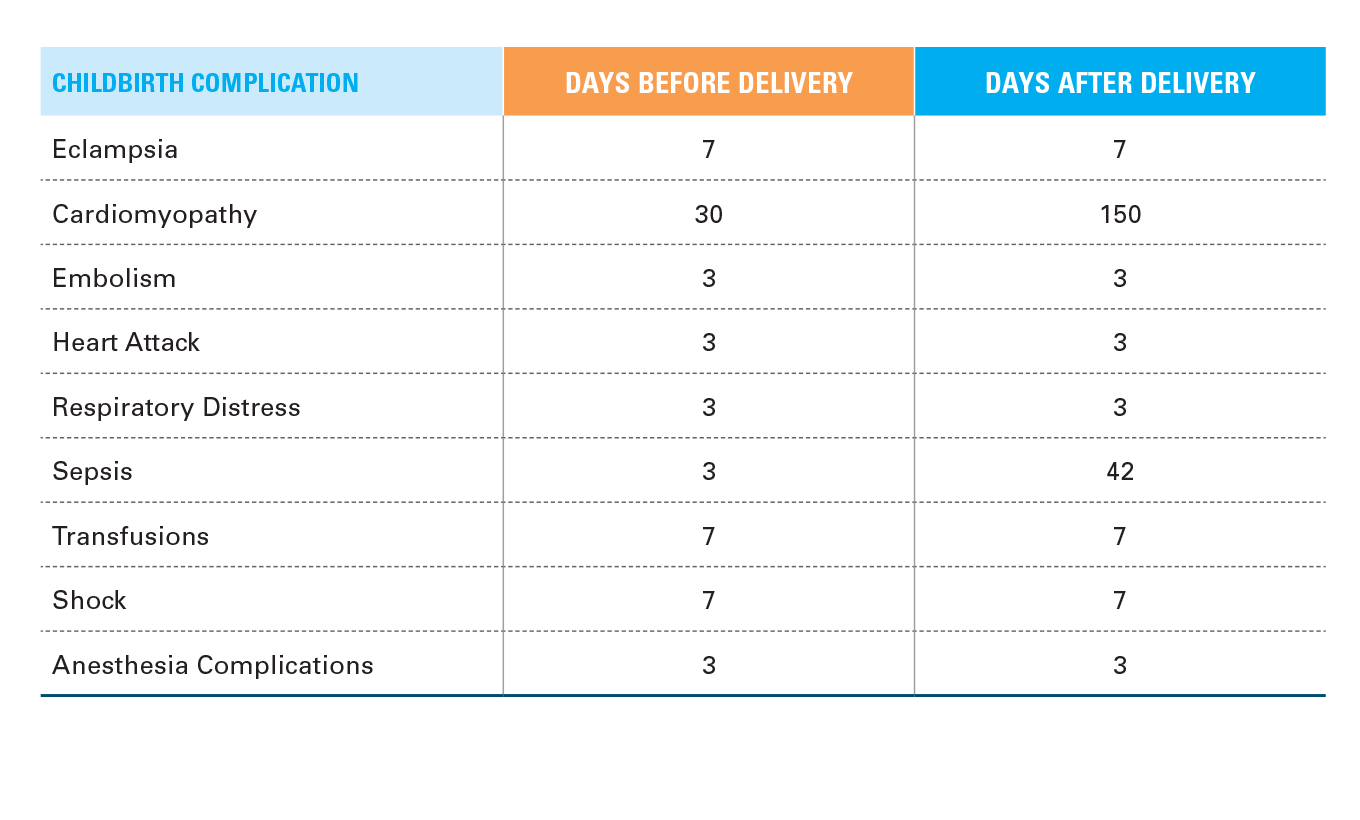
The complications studied were selected based on CDC information and input from clinical experts. Complications are divided into two groups based on when they occur during a childbirth episode. The analysis of pregnancy complications include gestational diabetes and preeclampsia. Childbirth complications include eclampsia, cardiomyopathy, sepsis, embolism, transfusions, heart attack, respiratory distress, shock, and anesthesia complications occurred within a certain window surrounding delivery (see Figure A below).
FIGURE A: TIME WINDOW USED FOR EACH CHILDBIRTH COMPLICATION
The chronic conditions studied include both behavioral health and physical health conditions. Behavioral health conditions focus on substance use disorders, anxiety and major depression that are highly associated with postpartum depression. Similarly, select physical health conditions focus on those that substantially increase the risk of pregnancy and childbirth complications such as hypertension and diagnosed obesity.
Endnotes
- This dataset includes only Blue Cross Blue Shield commercially-insured women, over 99% of whom were pregnant between the ages of 18-44.
- In April 2020, BCBSA surveyed >1,000 of commercially insured women 18-44 who were pregnant or delivered in March/April to understand the impact COVID has had on their mental health, prenatal care, postnatal care and delivery plans.
- BCBS Health Index data only goes back to 2014, thus we’re only able to examine prior health for women who were pregnant between 2015 and 2018.
- In January 2020, BCBSA surveyed >1900 commercially insured women, ages 18-44, who delivered a baby in the last 12 months and asked them about their utilization of prenatal and postnatal care.
- Pregnancy complications include gestational diabetes and preeclampsia. Childbirth complications include eclampsia, cardiomyopathy, sepsis, embolism, transfusions, heart attack, respiratory distress, shock, and anesthesia complications occurred within a certain window surrounding delivery.
- 2018 age distribution of pregnant women in the study: 18-24: 12.6%; 25-34: 61.0%; 35-44: 26.4%.
- Our data shows a dip in diagnoses of postpartum depression in 2016 followed by a rise. This trend is likely driven by two events: 1) the transition from ICD-9 to ICD-10 medical coding in 2015 and 2) in 2016, the U.S. Preventive Services Task Force recommended screening for depression in the general adult population, including pregnancy and postpartum women.
- A regression model was run on 2018 childbirth episodes to assess how each major factor drives cost, while controlling for other factors. Cost, the dependent variable, was regressed on the occurrence of pre-delivery complications (binary variable), the occurrence of delivery complications (binary variable), and whether the delivery was via C-section as opposed to vaginal (binary variable). Interaction terms between delivery method and occurrence of complications were included.
- Significance testing was applied and indicated statistical significance for the difference between Blue Distinction Centers and the national average for overall health of women, pregnancy complications and cost. There was no statistical significance for the difference in childbirth complications.
- BDC/BDC+ facilities care for women with a Health Index of 94.3, which is lower than the national average of 94.5. One point lower on the Health Index translates to an 8% increase in the impact of health conditions that could lower overall health.
- https://www.bcbs.com/blue-distinction-center/facility

